What is gastroschisis?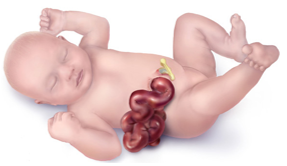
When a baby is developing in the mother, sometimes the skin of the abdomen does not close like it should. This leaves a hole in a baby’s abdominal wall. Some of the baby’s internal organs push through the hole and are outside the body when the baby is born (see picture). The intestines and sometimes the liver are outside of the baby’s abdomen. This is called gastroschisis.
What causes gastroschisis?
The cause of gastroschisis is not known. It happens in about 1 out of every 2,000 births. It happens most often in young mothers, and rarely occurs in mothers over 30. It is not related to anything the mother ate or did during pregnancy.
How is it diagnosed?
An ultrasound shows that the bowel and possibly the liver are outside of the baby’s body.
What other tests will be done during the pregnancy?
If your baby has gastroschisis, you will need more tests and monitoring than you would with a normal pregnancy. Babies with gastroschisis have an increased risk of dying before they are born.
Ultrasound. A baby with gastroschisis is often smaller than normal. Ultrasounds to watch your baby’s growth will be done at least each month.
Fetal movement counting. This will start at about the 28th week of your pregnancy. You will count your baby's movements one time every day, for a maximum of two hours. Your baby should move at least 10 times in 2 hours. If your baby moves 10 times in 10 minutes, you are done counting for that day. If your baby is not moving, call your doctor right away.
Non-stress tests and biophysical profiles. At around 32 weeks, non-stress tests will start. The non-stress tests are done once a week. Weekly biophysical profiles (BPPs) will start at the same time on alternating days.
Delivering your baby. Your baby’s delivery will be scheduled between the 35th and 38th week of pregnancy. Labor is usually induced. A vaginal delivery is preferred. A cesarean section is only done if there are other reasons.
How do you treat gastroschisis?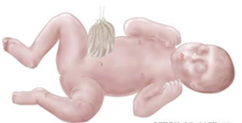
Right after birth, the lower half of your baby's body will be placed in a sterile bag. This is to hold moisture and heat in. Most babies will have surgery within several hours after birth.
Surgery is done to put the organs back inside your baby's abdomen. If possible, everything will be put back in at this time. This is called a primary closure. If the intestines do not all fit, we will place the exposed bowel in a sac (called silo.) The intestines will then gradually be put back into your baby’s abdomen.
The sac will be reduced daily or as your baby tolerates. We will close the abdominal wall once the entire bowel is in the abdomen.
Keeping pressure off the diaphragm. At delivery, we will place another tube into your baby's stomach. The tube will be placed either through the nose or mouth.
- Through the nose. This is a nasal gastric (NG) tube.
- Through the mouth. This is an oral gastric (OG) tube.
The tube keeps the stomach empty until the intestines are working.
What happens after surgery?
Help with breathing. After surgery, your baby may need help to breathe well. This is due to the increased pressure on the diaphragm from the bowels that are now in the abdominal cavity.
Placing IV and other lines. Your baby will not be able to eat for a while after surgery. Some special IV lines will be put in place while your baby is in the operating room for surgery.
- A central IV PICC line will be placed so we can give your baby vitamins, minerals, calories, and fat.
-
An arterial line may be placed in one of the arteries in the arm. This line lets us:
- Give IV fluid and medicines.
- Watch blood pressure.
- Take blood samples for lab work.
Drawing blood for testing. Blood samples will be taken often to test blood oxygen levels, electrolytes, blood count, and other things.
Medicines. Your baby may be on several medicines, including:
- Antibiotics to fight infection.
- Pain medicine to control pain.
Your baby may look puffy or swollen after surgery. The upper and lower legs may be very swollen. This is called edema. It will go away as your baby gets stronger and their body adjusts to the pressure of the bowels being back in the abdomen.
Providing nutrition. Babies with gastroschisis cannot eat for a long time. Special nourishment will be given through the central line. Total parenteral nutrition (TPN) is a solution that has protein, fats, sugar, vitamins, and minerals. TPN gives all the nutrition needed until your baby can take food by mouth.
What is my baby's long-term outlook?
Your baby will most likely not need any special care once you go home. Your baby's pediatric surgeon and pediatrician will provide the needed follow-up care.
Ask your doctor about tummy time for your baby.




