
Of Body and Mind: How Children’s Wisconsin Integrates Mental Health Into Every Aspect of Care
Greta never liked going to the doctor. No kid does, really. But for Greta, it was something different altogether. Anything from an annual checkup to taking cough medicine would nearly cause a panic attack. Thankfully, for most of her life, she was a happy, healthy kid and trips to the doctor were not a regular occurrence. But things took a turn when Greta was 8 years old.
One day in the fall of 2023, almost by chance, a family friend noticed something seemed off with how Greta was walking.
“She said, ‘This doesn’t look right. It looks painful,’” said Greta’s mom, Jenna. “But she never complained about pain. She has a very high pain tolerance. Or she just avoids it at all costs.”
At an annual appointment with Greta’s pediatrician not long after, the doctor recommended they go to the Children’s Wisconsin Orthopedics Program. An MRI revealed the issue.
Greta was diagnosed with spondylolysis with spondylolisthesis, a type of spinal defect that causes the vertebra of her lower back to slip out of normal position. She would need spinal fusion surgery to correct the issue.
Jenna knew this would be too much for Greta to handle. It was so serious, in fact, that in Greta’s health record it noted to not even mention the word “surgery” in her presence. Jenna asked the doctor if there was any mental health support he could recommend. That’s when they were put in touch with Nicholas Young, PhD, a Pediatric Psychologist who works with kids in the Children's Wisconsin Orthopedics Program.
Caring for the Whole Child
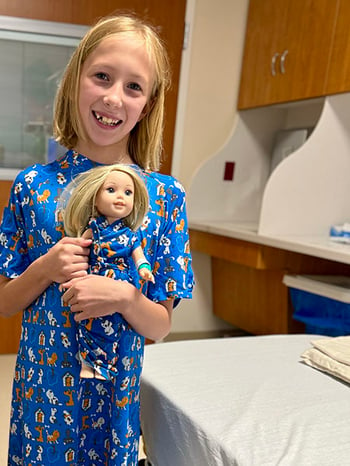 Even though Jenna asked for mental health support specifically, Dr. Young specifically sees every patient who is preparing for spinal fusion surgery.
Even though Jenna asked for mental health support specifically, Dr. Young specifically sees every patient who is preparing for spinal fusion surgery.
“Big surgeries can be hard on kids and families, so every patient who is going to have a spinal fusion comes to me for a pre-surgical health psychology evaluation,” said Dr. Young.
Dr. Young is part of the Pediatric Psychology team at Children’s Wisconsin. This team is made up of nearly 30 psychologists who specialize in helping children and families cope with and adapt to illness. At Children’s Wisconsin, pediatric psychologists are integrated into nearly every medical subspecialty, and into every area of the hospital — from cardiology, cancer, and orthopedics, to the PICU, CICU and NICU.
Kids with chronic health issues or those who experience a trauma-related injury are at higher risk for developing mental health issues. It can be anything from stress and anxiety over an upcoming surgery, fear of cancer coming back, self-esteem issues caused by physical differences, struggles keeping up or catching up with school, fitting in with peers or having to take responsibility for their own long-term care as they transition into adulthood. Children’s Wisconsin anticipates theses needs, and the Pediatric Psychology team brings that care directly to the patient.
“Patients with chronic medical conditions are at higher risk for anxiety and depression,” said Cheryl Brosig Soto, PhD, Division Chief of Pediatric Psychology and Developmental Medicine at Children’s Wisconsin. “In addition, patients with certain medical conditions, such as complex congenital heart disease, those born with extreme prematurity or those who are long-term cancer survivors are at higher risk for neurocognitive issues.”
Pediatric psychologists who consult within the hospital and are embedded in medical specialties have unique expertise in those specialty-specific conditions that other more general mental health providers in the community might not have. They understand the medical treatment and the sometime complex medical recommendations that patients and families are expected to follow.
“Pediatric psychologists have been integrated into medical teams at Children’s Wisconsin for more than 30 years,” said Dr. Brosig Soto, who is also Professor of Pediatrics at the Medical College of Wisconsin, the academic partner of Children’s Wisconsin. “It has been exciting to see the growth of our team and how our medical colleagues have embraced the integrated health model. Much of my time now is spent recruiting more psychologists, as additional medical specialties are asking for psychologists to be part of multidisciplinary clinics.”
Putting in the Work
 For Dr. Young and the Orthopedics Program specifically, a central goal for these sessions is to identify and manage any behavioral health factors that may impact the surgery and recovery. Pain is a common concern in surgery, especially orthopedics. Recovery and rehab can often be painful, and pre-existing anxiety or depression can make it worse. People can build it up so much in their head — catastrophizing it, Dr. Young said — that they’ll avoid their rehab, which will prolong their recovery, extend their hospital stay and delay their return to normal life.
For Dr. Young and the Orthopedics Program specifically, a central goal for these sessions is to identify and manage any behavioral health factors that may impact the surgery and recovery. Pain is a common concern in surgery, especially orthopedics. Recovery and rehab can often be painful, and pre-existing anxiety or depression can make it worse. People can build it up so much in their head — catastrophizing it, Dr. Young said — that they’ll avoid their rehab, which will prolong their recovery, extend their hospital stay and delay their return to normal life.
Greta had almost the exact opposite concern. Hospitals scared her so much that she endured her pain in silence, knowing if she acknowledged it and spoke up she’d likely have to go to the doctor.
“Under communicating pain is a big consideration,” said Dr. Young. “It's a different form of catastrophizing. Like if your brain allows you to think about it and make it real, it’ll bring about that scariness. But if they're not communicating what their pain-related needs are, then these poor kids can suffer in silence and not get the help they need. And that's pretty much the exact opposite of what we want to do.”
Dr. Young and Greta hit it off instantly. They bonded over his colorful shoes (they were pink Nikes so Greta started calling him Dr. Pinkalicious) and their shared love of “Bluey.” They even had the same favorite episode: “Unicorse.”
After the initial getting-to-know-each-other goofiness, Dr. Young began to work with Greta to prepare her for surgery. During five visits over two months, Dr. Young utilized several different tools to help Greta manage her anxiety.
He taught her breathing exercises that she could use in the moment to help calm her body down — “hot chocolate breathing,” they called it. They made a storybook together that walked through every small step of the surgery, so Greta knew exactly what to expect.
“It covered everything from when we arrived in the morning, what they’re going to do, how they take her to the operating room, she’ll breathe in the medicine and go to sleep and when she wakes up mom and dad will be there,” said Jenna. “The story was key.”
“It's a fantastic tool because it takes the mystery out of it,” said Dr. Young. “It gets them to face the fears. Instead of being stressed out in your head where those anxious thoughts are very disorganized, it puts it on paper into a product that you can look at and get a lot more comfortable with. Plus, making it is fun.”
Dr. Young also encouraged Greta to take some smaller steps to help get her out of her comfort zone as practice.
“For some people, doing something new can be exciting and thrilling,” said Dr. Young. “But for a lot of people it's scary, especially when you're at that young of an age.”
“Greta’s favorite place to eat is Culver's,” said Jenna. “So, Dr. Young suggested we go to Culver’s but I would order something for Greta as a surprise. Instead of her usual cheeseburger, maybe I’d get her chicken tenders or a grilled cheese, or even a different flavor of ice cream. Small things like that to help her break out of her structure a bit.”
When the day of the surgery arrived — Aug. 31, 2024 — Greta walked into the hospital with a smile.
“She wasn’t scared at all. Dr. Young made a 100% difference,” said Jenna. “She said it was fun.”
Greta saw Dr. Young two weeks after her surgery and then one last time a few months later.
Today, Greta is doing great. While she’s facing some other health issues, thanks to her care team at Children’s Wisconsin and the skills she learned from Dr. Young, she’s not letting them overwhelm her. She’s very much your typical, active and caring 10-year-old girl. She loves reading, crafting, hiking, singing and playing the guitar. She loves the Beatles and “Hamilton.” And when things start to get hard, she always has her “hot chocolate breathing.”
“I always tell families that I want to work myself out of a job,” said Dr. Young. “We want you to get back to normal life as fast as reasonably possible. Greta did so well, better than expected. Her anxiety went from very high to a place that we would expect for a kid of her age. It was so rewarding to see that. But the credit does go to her and her family for doing all the work. I was the guide, but they were in the trenches day to day, practicing, rehearsing, modeling and doing it together as a family.”
Commitment to Mental Health
 The Pediatric Psychology team is part of a larger mental and behavioral health focus at Children’s Wisconsin.
The Pediatric Psychology team is part of a larger mental and behavioral health focus at Children’s Wisconsin.
“Children’s Wisconsin has made a commitment to pediatric mental health and integrating it into care,” said Dr. Brosig Soto. “We’ve invested a lot in this over the last five years.” In fact, since 2019, Children’s Wisconsin has provided more than $150 million to improve mental health services for kids in Wisconsin. The main pillars of that investment include identifying concerns sooner, improving access to care and reducing stigma around both mental illness and mental health care.
“There can be a lot of stigma that comes along with mental health,” said Dr. Young. “Making it a standard part of care helps normalize it for patients.”
Dr. Brosig Soto agrees. And she knows removing that barrier is a vital step to ensuring all kids get the care they need, when they need it.
“By integrating mental health into specialty care, the psychologist is considered part of the team. That helps make it more accepted by families and the patients,” she said. “At Children’s Wisconsin, we don’t just believe that mental health is health, we know it is.”
Children's Wisconsin Resources

Written by
Writer
Related Stories
No related articles found.
