
Guiding Lights: Finding Support and Connection in the NICU
In the early days of Alayna’s long stay in the Children’s Wisconsin Neonatal Intensive Care Unit (NICU), her mother, Ai, isolated herself in the darkness of Alayna’s hospital room, still reeling from the shock of her baby’s premature and dramatic start to life.
“I was not emotionally or mentally ready to do anything besides stay with my baby,” said Ai.
But Alyssa Voigt, a NICU Family Support Coordinator, and the nurses kept checking in, reminding Ai to take care of herself, too. Ai took some baby steps — first observing as other NICU mothers crafted and chatted while she ate her lunch in the family room, responding to their friendly questions about her baby. After a few more lunches, she joined them for craft projects. Before long, Ai was the one urging other mothers to leave their baby’s bedsides for a brief break and reassuring them when they were worried.
“I loved it,” Ai said of those early connections. “I got to meet other mothers and hear their stories, their experiences.”
The NICU Family Support Program is made possible because of the longstanding partnership between Children’s Wisconsin and the March of Dimes, a nonprofit dedicated to supporting the health of moms and babies. Alyssa serves as a liaison between families and hospital staff, provides education and tries to bring comfort and joy into what can be a stressful environment. That means everything from organizing twice-weekly craft-making gatherings for NICU families to giving personalized gifts to bring a smile to weary parents’ faces.
“A big part of it is just connecting parents, having that shared experience and being able to talk it through with someone who actually understands in real time what they’re going through,” said Alyssa, a former NICU mom herself.
The NICU “Roller Coaster”
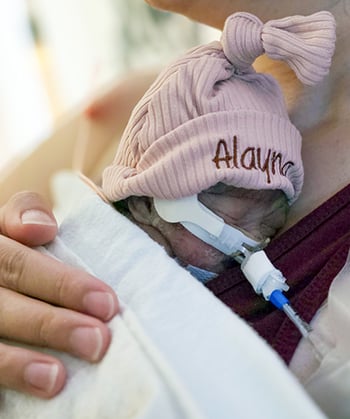 The support was invaluable to first-time parents Ai and her husband, Kou. About 24 weeks into Ai’s pregnancy, the couple learned Ai had placental abruption, a serious pregnancy complication that can affect the baby’s oxygen and nutrient levels. Ai’s cervix was also dilated, indicating that Alayna’s arrival could be much sooner than expected.
The support was invaluable to first-time parents Ai and her husband, Kou. About 24 weeks into Ai’s pregnancy, the couple learned Ai had placental abruption, a serious pregnancy complication that can affect the baby’s oxygen and nutrient levels. Ai’s cervix was also dilated, indicating that Alayna’s arrival could be much sooner than expected.
The plan was to keep Ai on bedrest to postpone delivery as long as possible, but Alayna had other plans — and had shifted into a feet-first breech position. Alayna was delivered via an emergency Cesarean section at a hospital in Green Bay on July 18, 2025, 15 weeks ahead of schedule. At just 1 pound, 8 ounces, she reminded her parents of a tiny doll.
Soon after, Alayna developed an infection, and she needed more advanced care than the local NICU could provide. That was when Kou and Ai put their newborn daughter in an ambulance to the Children’s Wisconsin Milwaukee Hospital, home to the state’s largest Level IV NICU.
At Children’s Wisconsin, the infection was only the first hurdle Alayna faced, from blood clots in her brain to liver issues to feeding and breathing challenges. Doctors eventually determined that Alayna had patent ductus arteriosus (PDA), a common heart condition in premature infants in which a fetal blood vessel remains open instead of closing as usual. After a catheter procedure corrected the PDA, Alayna’s eating and breathing improved.
“It’s definitely a roller coaster,” Kou said of the NICU experience. “You have your lows and then you have your highs.”
Another concern was necrotizing enterocolitis (NEC), a severe intestinal disease that can affect preemies. When Alayna first arrived at Children’s Wisconsin, her abdomen was blue and bloated, which can be a sign of NEC.
“That scared me because I heard so many things about NEC,” said Ai, who eventually had to stop watching NICU stories on TikTok because it only added to her stress. She and Kou were relieved when NEC was ruled out.
A Higher Level of Neonatal Care
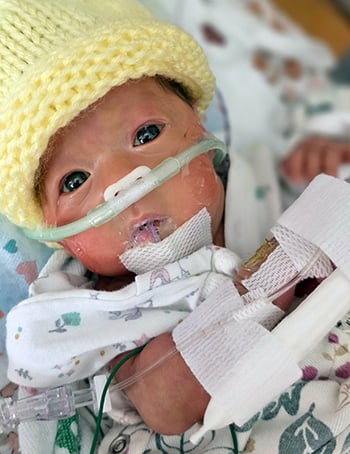 But despite the ups and downs, Ai and Kou were grateful that they had transferred Alayna to Children’s Wisconsin. They initially assumed a NICU was a NICU, but they immediately noticed a difference at the Milwaukee Hospital. They were impressed by the large, multidisciplinary teams, daily huddles and deep expertise of the nursing staff, as well as the collaboration and mutual respect they observed between doctors and nurses. They also appreciated that Children’s Wisconsin is an academic medical center, where medical students, interns and residents train under expert specialists.
But despite the ups and downs, Ai and Kou were grateful that they had transferred Alayna to Children’s Wisconsin. They initially assumed a NICU was a NICU, but they immediately noticed a difference at the Milwaukee Hospital. They were impressed by the large, multidisciplinary teams, daily huddles and deep expertise of the nursing staff, as well as the collaboration and mutual respect they observed between doctors and nurses. They also appreciated that Children’s Wisconsin is an academic medical center, where medical students, interns and residents train under expert specialists.
“You can see the difference in the level of care and knowledge,” said Kou. “The nurses have a lot of experience and are willing to advocate for you. The doctors are great, very knowledgeable, and they’re educators too, which is a huge plus.”
Pediatric Neonatologists Scott Welak, MD, and Ru-Jeng Teng, MD, played an important role in Alayna’s care early on. Pediatric Neurologist Samuel Adams, MD, also quickly won the family’s trust and respect.
“Everyone was a team,” said Ai. “Everyone listened and really was trying to find the best route for Alayna.”
Alayna’s primary nurse, Kaye Koehoorn, was a constant source of positivity and encouragement, reassuring them, “You’re at Children’s Wisconsin. She’s going to be fine.”
“It made us feel more at ease,” said Ai.
Alyssa and the NICU Family Support Program made sure Ai and Kou’s needs were met, too. The hospital’s social workers, psychologists and chaplains conduct regular “psych-social rounds” to discuss the well-being of each NICU family. “The health of the baby is drastically improved by the health of the family,” said Alyssa.
Before Kou’s birthday, Ai asked Alyssa for help making Kou a birthday card from Alayna. Knowing that Kou is an avid runner, Alyssa and Kaye crafted a running-themed poem titled: “To My Marathon Dad: From Your Tiniest Teammate.” The opening lines read:
“Happy Birthday, Daddy — I see you near,
Though wires and beeps are all I hear.
I’m running my race from this tiny bed,
But your love surrounds me, just like you said.”
Adjusting to Life at Home
 Alayna was finally discharged on Halloween 2025, just one day after her original due date. She continues to be monitored by the DREAM (Developmentally Ready: Engagement and Achievement of Milestones) Clinic and other specialists at Children’s Wisconsin, and she is growing and developing well. She even decided to end her supplementary oxygen ahead of schedule, pulling out her oxygen cannula overnight. Fortunately, her pulse oximeter readings showed that she remained stable without the oxygen support.
Alayna was finally discharged on Halloween 2025, just one day after her original due date. She continues to be monitored by the DREAM (Developmentally Ready: Engagement and Achievement of Milestones) Clinic and other specialists at Children’s Wisconsin, and she is growing and developing well. She even decided to end her supplementary oxygen ahead of schedule, pulling out her oxygen cannula overnight. Fortunately, her pulse oximeter readings showed that she remained stable without the oxygen support.
“She’s been the boss, basically,” said Kou.
And while Ai and Kou appreciated the expertise and support of the NICU, they are grateful to finally settle into a quieter life at home. And so, apparently, is Alayna.
“Alayna loves not being touched every minute, every hour,” said Ai. “She loves to be able to sleep, to be able to just be a baby.”
Children's Wisconsin Resources

Written by
Writer
Children's Wisconsin specialty care providers have advanced training and expertise in many areas of pediatric medical care, including allergies, dental, dermatology, emergency medicine, ENT, gastroenterology, neonatology, surgery and more.
Related Stories
No related articles found.
