On October 24, 2019, something of a miracle happened. Bri Bernhardt and Nick Reid discovered they were going to have a baby. Their respective ages and Nick’s past cancer treatment left that possibility very much in doubt. But the blood test didn’t lie. On July 3, 2020, they would be parents.
 “We were in shock and over the moon. Just speechless,” said Bri. “It was one of those moments where you get tunnel vision. We couldn’t believe it actually happened. Like we hit the lottery.”
“We were in shock and over the moon. Just speechless,” said Bri. “It was one of those moments where you get tunnel vision. We couldn’t believe it actually happened. Like we hit the lottery.”
But exactly two weeks later, all their excitement and hope and joy came crashing down. They received more shocking and unexpected medical news: Bri had cancer.
A biopsy on a mole she had on her hip for years came back positive for melanoma. Doctors told her a quick surgical removal should take care of it.
“At first I thought, ‘Okay, I’m going to be fine. They’re going to cut this thing out and life will go back to normal,’” said Bri.
But a swollen lymph node in her groin discovered a couple weeks later revealed that the cancer had spread and was more advanced and aggressive than originally thought. The two excited parents-to-be were now faced with an impossible choice.
“In an instant, we were thrust into the greyest of areas from not only a medical standpoint, but also our own morals,” said Nick. “We faced a myriad of decisions, the foremost being what to do with this budding life.”
Uncharted territory
 Despite its more advanced nature, the doctors all agreed Bri’s cancer could be treated effectively with surgery and immunotherapy, a newer type of cancer treatment that uses a person’s own immune system to destroy cancer cells. But what they were less sure of was what effect the treatment would have on her pregnancy. The baby was likely to have birth defects, but to what degree no one could say for sure.
Despite its more advanced nature, the doctors all agreed Bri’s cancer could be treated effectively with surgery and immunotherapy, a newer type of cancer treatment that uses a person’s own immune system to destroy cancer cells. But what they were less sure of was what effect the treatment would have on her pregnancy. The baby was likely to have birth defects, but to what degree no one could say for sure.
In the United States, there have only been a handful of cases where a pregnant woman was treated with immunotherapy. In all cases, the baby was born with some level of birth defect or complication, ranging from low birth weight to reduced thyroid function. Preterm delivery is another concern and, in some cases, the fetus didn’t survive.
“Because the treatment is so new, there is limited data on the effects of immunotherapy on a human fetus. We do know the targets of the treatment are found in the placenta and certain medications can be transmitted to the fetus through the placenta,” said Amy Harker-Murray, MD, Bri’s oncologist with Froedtert & the Medical College of Wisconsin Clinical Cancer Network. “For these reasons, immunotherapy is not recommended in pregnancy and any use requires a very thoughtful, in-depth, risk-benefit discussion with a pregnant patient.”
But it wasn’t just the treatment they had to be concerned about. Bri’s specific type of cancer posed a unique risk, as well. Melanoma is a cancer that can most easily be passed onto a growing fetus. The possibility that their baby would actually be born with cancer was a very real one.
“While a situation where a cancer can potentially spread through the placenta to the fetus in utero is very rare, malignant maternal melanoma has the highest likelihood of transmission among all types of cancers,” said Vijender Karody, MD, a neonatologist in the Children’s Wisconsin Neonatal Intensive Care Unit (NICU).
The overall rate for any birth defect is about 1 in every 33 babies. A mom spreading cancer to her fetus is around 1 in 1,000. But of those reported cases of fetal transmission, melanoma accounts for 31 percent.
“We don’t exactly know why this is,” said Dr. Karody, who is also an associate professor of neonatology at the Medical College of Wisconsin. “It’s hypothesized that melanoma cells can alter their genetic makeup before they spread through the placenta so that the fetus’ immature immune system doesn’t recognize them and respond.”
Undeterred, Bri and Nick knew they wanted to continue with the pregnancy and they would do whatever they could to protect the fetus. At that point, Bri’s OB-GYN at a nearby Milwaukee hospital instructed her there was only one place that could handle her unique situation: Children’s Wisconsin.
“It was our decision ultimately, but the doctors that we talked to from Children’s Wisconsin said, ‘Let’s go for it,’” said Bri. “They did a balancing act between treatments and monitoring the pregnancy so they could minimize those risks and Bri could still have a relatively normal life.”
A balancing act
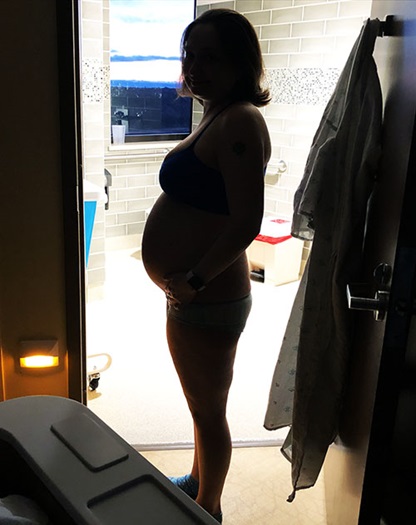 Bri started treatment right away at Froedtert and elected to have all the lymph nodes from her right groin surgically removed with nothing more than a spinal block and Tylenol for the pain. She then began receiving monthly infusions of immunotherapy. All the while, Zachary Colvin, MD, Bri’s new OB-GYN at Froedtert who is also a maternal fetal medicine specialist at the Children’s Wisconsin Fetal Concerns Center, coordinated everything between the two hospitals to help strike that delicate balance of Bri’s health and the baby’s development.
Bri started treatment right away at Froedtert and elected to have all the lymph nodes from her right groin surgically removed with nothing more than a spinal block and Tylenol for the pain. She then began receiving monthly infusions of immunotherapy. All the while, Zachary Colvin, MD, Bri’s new OB-GYN at Froedtert who is also a maternal fetal medicine specialist at the Children’s Wisconsin Fetal Concerns Center, coordinated everything between the two hospitals to help strike that delicate balance of Bri’s health and the baby’s development.
“We went into this treatment knowing that at any moment Bri could lose the pregnancy, have catastrophic birth defects or, worst of all, lose her own life,” said Nick.
1
Fast forward to May 1, 2020. Bri is now 31 weeks pregnant and visiting with Dr. Colvin and Dr. Harker-Murray. Everything looked great. The baby’s weight had increased and was officially in the “normal range” while Bri’s MRI and labs showed no evidence of cancer. The pregnancy was in its home stretch. But as the two were in their car about to leave the hospital parking structure, suddenly and without warning Bri lost consciousness and began having a violent seizure.
Thankfully, a nurse was passing by and immediately called 911. Bri was rushed to the ER. There they received even more devastating news: The cancer had spread to her brain.
What role Bri’s pregnancy had on the growth and spread of her cancer is difficult to pinpoint. While some doctors believe there may be a connection between pregnancy and cancer growth, it has not been firmly established.
“Some cancers have hormone receptors on them. If the cancer has a hormone receptor, and that hormone is increased in pregnancy, that cancer is likely to grow during pregnancy,” said Meghen Browning, MD, a pediatric hematologist-oncologist at the MACC Fund Center for Cancer and Blood Disorders at Children’s Wisconsin. Dr. Browning, who is also an assistant professor of pediatric oncology at the Medical College of Wisconsin, reviewed the baby’s lab results and records. “In theory, all the ‘growth signals’ that help develop a fetus could also promote cancer growth, but that is a pretty non-specific thing to say, and most cancers do not appear to grow faster during pregnancy.”
Another impossible decision
 Once Bri was stabilized, she and Nick faced another crucial, impossible decision. Continue the pregnancy with limited treatment for Bri or deliver the baby early to allow for more aggressive cancer therapies.
Once Bri was stabilized, she and Nick faced another crucial, impossible decision. Continue the pregnancy with limited treatment for Bri or deliver the baby early to allow for more aggressive cancer therapies.
“It was one of the hardest decisions we’ve had to make,” said Bri. “We opted to have the baby.”
At 9:44 a.m. on May 4, 2020, Brianna Jr. was born. She was immediately taken down the adjoining hallway from the Froedtert Hospital Birth Center to the Children’s Wisconsin NICU.
“It was a unique case, a learning opportunity for the entire unit,” said Dr. Karody. “I’ve been practicing for more than 10 years and this was the first such case I’ve seen.”
Thinking they had more time before the baby would be born, Bri and Nick hadn’t yet decided on a name. They chose Brianna Jr. as a temporary fill in, but the name has since stuck. And what better way to honor Bri, all she went through and the sacrifices she made to ensure Brianna Jr. was able to be born as healthy as possible.
 As healthy as possible. Now it was time to see how healthy she actually was, to face the fear that had haunted Nick and Bri’s thoughts every day since their journey started. What effect did Bri’s cancer treatment have on her? What defects was she born with? Did she have cancer herself?
As healthy as possible. Now it was time to see how healthy she actually was, to face the fear that had haunted Nick and Bri’s thoughts every day since their journey started. What effect did Bri’s cancer treatment have on her? What defects was she born with? Did she have cancer herself?
In her first few weeks of life, Brianna Jr. was examined thoroughly by Dr. Karody as well as by specialists from the MACC Fund Center for Cancer and Blood Disorders and the Dermatology Program. She had blood tests and ultrasounds. Bri’s placenta was biopsied and tested. The two new parents nervously awaited word.
Nothing. They found nothing. Every test that was run, every exam that was conducted came back negative. According to Dr. Browning, Brianna Jr. has no sign of cancer or any side-effects from Bri’s treatment.
“Brianna Jr. is an incredible success story and she really exemplifies what’s possible with the right medical team in place,” said Nick. “She’s absolutely perfect in every sense of the word. Our lives have immediately taken on a new meaning.”
Nothing is guaranteed
 For the next six weeks, Brianna Jr. was cared for by a whole team of NICU doctors, nurses, therapists and other support staff — more names than Bri and Nick can recall but whose love, comfort and support they’ll never forget.
For the next six weeks, Brianna Jr. was cared for by a whole team of NICU doctors, nurses, therapists and other support staff — more names than Bri and Nick can recall but whose love, comfort and support they’ll never forget.
Meanwhile, Bri resumed her cancer treatment. One week after giving birth, she underwent surgery to remove the two tumors that had developed in her brain. A few weeks later, she started a more aggressive round of targeted therapy.
Another unfortunate side effect of Bri’s cancer treatment was she wasn’t able to breastfeed Brianna Jr., something she had desperately wanted to do. It just wouldn’t be safe. But the lactation team at Children’s Wisconsin was able to provide her with donated human breast milk so Brianna Jr. could have the next best thing to Mom’s.
Juggling her own care and treatment with her new baby was a lot — sometimes too much. But the nurses in the NICU took incredible care of Brianna Jr. And with the help of the AngelEye webcams, Bri was always able to check in on her baby girl, even if she wasn’t well enough to visit in person. Knowing Bri’s cancer journey, the NICU nurses would often leave words of encouragement for her to read through the webcam.
Being able to see her baby every day — and knowing how the whole team was thinking of her and rooting for her — gave Bri all the strength and motivation she needed to push through those hardest days. She has about a year of treatment ahead of her and much remains unknowable, but she and Nick and her doctors are remaining optimistic.
 As for Brianna Jr., she made remarkable progress. Despite arriving more than two months early, she was soon breathing on her own, feeding well and hitting every milestone.
As for Brianna Jr., she made remarkable progress. Despite arriving more than two months early, she was soon breathing on her own, feeding well and hitting every milestone.
“If you didn’t know Mom’s history, you would never suspect anything,” said Dr. Karody. “Brianna Jr. had a very typical course for a preemie, which given the circumstances, was the best case scenario anyone could have hoped for.”
With that positive growth and development coupled with her mom’s uncertain health, on the evening of June 12, more than three weeks ahead of schedule, doctors decided Brianna Jr. was ready to go home.
For the foreseeable future, she will be followed closely by Valerie Carlberg, MD, from the Children’s Wisconsin Dermatology Program to make sure she remains cancer-free. And Karen Swanson, MD, a pediatrician at the Children’s Wisconsin Pewaukee Pediatrics primary care office, will monitor her growth and development as she would any other healthy baby. But despite the long, difficult journey, Bri and Nick are beyond grateful to have their baby girl and spend as much time as they possibly can together.
“Nothing in this life is guaranteed,” said Nick. “Bri and I searched for each other our entire lives, sacrificed everything we knew to start a new life together and learned the true meaning of our ‘sickness and health’ vow. Don’t ever take those who you love for granted.”







