Thanks to our generous partners at the MACC Fund, Northwestern Mutual and the Gold In September (G9) Program of Beat Childhood Cancer, we can provide innovative research to help kids like Yasmeen.
Just as Ivan pulled his family's black SUV into the driveway of his mother-in-law’s suburban Chicago home on a cool October day in 2005 — his wife, Judy, by his side, their 2-year-old daughter, Yasmeen, buckled in the back — his phone rang. While Judy picked Yasmeen up from her car seat, a small tan Band-Aid still on her arm covering the needle prick that had drawn her blood not even an hour earlier, Ivan answered the call without hesitation.
Ivan knew who was on the other side of that phone and that the information he had could potentially change their lives forever. As Judy carried Yasmeen up to the house, Ivan trailed a few steps behind with the phone pressed to his ear, listening and absorbing, as best as he could, what the doctor was telling him.
It had all started a day earlier. Ivan and Judy noticed some curious bruising on Yasmeen’s arms and legs. At first they just thought they were from rough housing with her older cousins, but when they noticed some on her face, as well, they grew concerned.
“She also just wasn’t herself,” said Ivan. “Just lethargic, not her usual, happy self.”
They took Yasmeen to her primary care physician and Ivan could tell right away he was alarmed. He sent Yasmeen to get blood work done at a hospital near their home in Willowbrook, Illinois. Now, the results were in. On the phone, the doctor told him there was a high concentration of blast cells in Yasmeen’s blood. Blast cells are immature white blood cells and a higher than normal number of them, the doctor explained, indicates leukemia. He told Ivan to take Yasmeen to Loyola University Medical Center immediately.
As Ivan shut the door, he broke the news to his wife and mother-in-law. Outwardly, for Yasmeen’s sake, they kept their calm composure, not letting the hurricane of fear and shock swirling inside them show on their faces.
“To be honest, we were devastated,” said Ivan. “We didn’t know what to think, what this means. We didn’t know anything.”
The first round
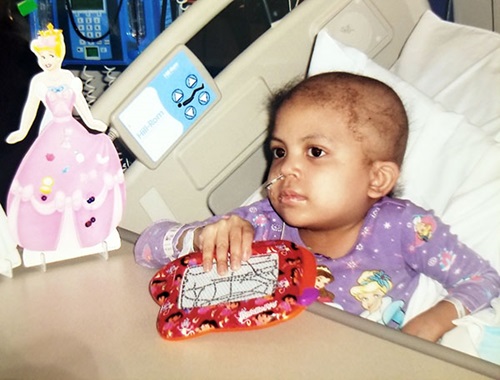 Yasmeen’s official diagnosis was acute lymphoblastic leukemia. This cancer of the blood and bone marrow — the most common type of childhood cancer — attacks the white blood cells, damaging the person’s immune system. Though serious, it is treatable, with about 98 percent of children going into remission and 90 percent remaining so after 10 years. Yasmeen immediately started a two-and-a-half-year course of chemotherapy at Loyola.
Yasmeen’s official diagnosis was acute lymphoblastic leukemia. This cancer of the blood and bone marrow — the most common type of childhood cancer — attacks the white blood cells, damaging the person’s immune system. Though serious, it is treatable, with about 98 percent of children going into remission and 90 percent remaining so after 10 years. Yasmeen immediately started a two-and-a-half-year course of chemotherapy at Loyola.
Flash forward to November 2007. After nearly two years of treatment, coming to the hospital several times a month — even daily at some points — Yasmeen seemed to be doing well. Until one day, she wasn’t. A routine blood test at one of her appointments showed the cancer was back.
“In our minds, things were going well. We just had a few more months of treatment left and we were getting ready to put this all behind us,” said Judy. “So, we were very surprised, shocked. We didn’t understand.”
1
Since she relapsed before finishing the initial treatment, her oncologist told them a bone marrow transplant would give Yasmeen the best chance of recovery. And the best place to go, he said, was Children’s Wisconsin.
“He talked highly of the communication and the services his patients were getting at Children’s Wisconsin,” said Ivan. “We wanted to give her the best chance, so we decided to make the trip.”
The family packed up the car and made the 90-minute drive to Milwaukee and started the long treatment process over again, now under the care of Julie Talano, MD, a pediatric hematologist/oncologist/bone marrow transplant physician in the MACC Fund Center for Cancer and Blood Disorders at Children’s Wisconsin.
The first step was finding a donor. The best chance for a match is a full biological sibling, so Yasmeen’s younger sister was tested. Unfortunately, she was not a full match. The search then branched out to unrelated donors in the National Marrow Donor Program. After about a month, a suitable donor was finally identified through the Be The Match registry. In late February 2008, Yasmeen was admitted to the hospital to start her week-long pre-transplant chemotherapy and radiation — her own immune system first had to be wiped out before her body could accept the bone marrow transplant.
On March 9, 2008, Yasmeen received her transplant.
She was 4 years old.
Running out of options
 For the next eight months following the bone marrow transplant, Yasmeen, again, seemed to be doing well. But, once again, things took a sudden and unexpected turn. At a routine follow-up appointment at Children’s Wisconsin in January 2009, her blood work once again showed the presence of abnormal cells.
For the next eight months following the bone marrow transplant, Yasmeen, again, seemed to be doing well. But, once again, things took a sudden and unexpected turn. At a routine follow-up appointment at Children’s Wisconsin in January 2009, her blood work once again showed the presence of abnormal cells.
This time, Yasmeen was diagnosed with myelodysplastic syndrome, a serious condition in which blood cells don’t develop properly, and she was showing early signs of relapse. A second bone marrow transplant was recommended, which Yasmeen received on May 27, 2009. The previous donor wasn’t available this time but they were able to find an umbilical cord blood donation.
Now 5 years old, Yasmeen had spent more than half her life battling cancer.
Unlike the previous two treatments, however, Yasmeen did not initially do well. Just a few days following her second transplant, Yasmeen’s condition took a dire turn.
Yasmeen had developed acute graft-versus-host disease, a potentially serious complication in bone marrow transplant patients. When this happens, the immune system of the donor cells identify the patient’s body as foreign and attack it as it would a virus or infection. Of the approximately 18,000 bone marrow transplants that occur every year, as many as half will develop graft-versus-host disease to some degree. Yasmeen’s was grade 4, the most serious kind.
“Her skin was literally peeling and her intestines were bleeding quite a bit,” said Ivan. “She was bedridden.”
Typical treatments — such as steroids and immune suppressive medication — weren’t working, so Yasmeen was transferred to the Children’s Wisconsin Intensive Care Unit as doctors struggled to find an effective treatment.
“For Yasmeen, the same bone marrow transplant cells meant to save her from leukemia also attacked her own gastrointestinal tract, leading to life-threatening bleeding. She required multiple medications given continuously to try to control her bleeding and her blood pressure,” said Rebecca Bertrand, MD, a critical care physician at Children’s Wisconsin who oversaw Yasmeen’s care in the ICU. “Because of the severity of her blood loss, she was dependent on frequent transfusions of blood, plasma and platelets to stay alive.”
That’s when Dr. Talano, who is also a professor of pediatric hematology and oncology at the Medical College of Wisconsin, recommended a new, experimental treatment.
Putting faith in the future
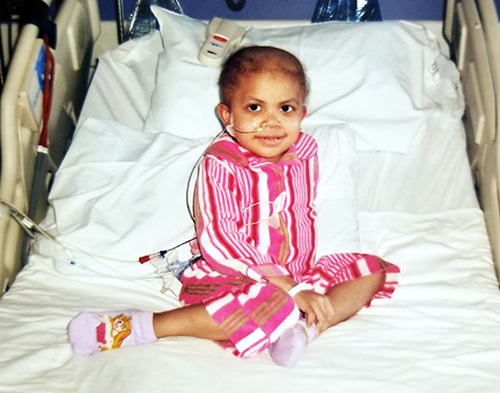 Dr. Talano told Ivan and Judy about this new treatment she was familiar with that used mesenchymal stem cells to help fight back against the graft-versus-host disease.
Dr. Talano told Ivan and Judy about this new treatment she was familiar with that used mesenchymal stem cells to help fight back against the graft-versus-host disease.
“Mesenchymal stem cells are found in a person’s bone marrow and they have unique properties where they help dampen the immune response,” said Dr. Talano. “They also go to areas of inflammation and help with tissue repair.”
These cells are harvested from a healthy donor and then multiplied and turned into a medicinal treatment. While the therapy was still in the clinical trial phase and had not yet been approved by the FDA — Dr. Talano was leading a trial at Children’s Wisconsin and had used it on a few other patients — it had been approved for “compassionate use” in cases where all other treatment options have failed. Yasmeen certainly qualified.
“We were very fearful of an experimental treatment, but there was no better choice available,” said Judy. “We went back and forth with it but we decided to do it. We put our faith in it.”
2
Yasmeen started treatment right away, receiving hour-long transfusions twice a week for the first four weeks, then once a week for an additional four weeks.
Her condition improved almost immediately.
“We were both relieved and surprised with how well Yasmeen responded,” said Ivan. “We saw positive results right away. All of a sudden, she perked up.”
“It worked remarkably well for Yasmeen,” said Dr. Talano. “It saved her life.”
Hope through research
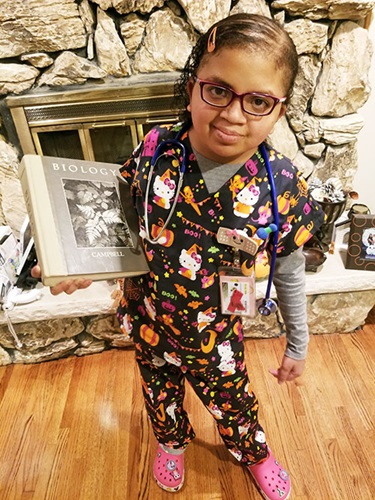 About a week after starting the mesenchymal stem cell treatment, Yasmeen was stable enough to be transferred back to the MACC Fund Center, just in time for her 6th birthday on June 11.
About a week after starting the mesenchymal stem cell treatment, Yasmeen was stable enough to be transferred back to the MACC Fund Center, just in time for her 6th birthday on June 11.
And on Sept. 22, 2009, Yasmeen was ready to head home. With a mix of excitement and fear, after four months at Children’s Wisconsin, Ivan and Judy took their daughter home to Chicago. And while they couldn’t know for sure what the future held, what they did know for a fact was Yasmeen was given another chance at life, thanks to this experimental treatment and the faith they put in Dr. Talano.
“A lot of doctors and hospitals weren’t even aware of this treatment because it wasn’t approved,” said Ivan. “But Dr. Talano, because of her level of experience and the research she had been working on, it was a tool she was aware of.”
The world of medicine is constantly evolving and as the region's only independent health care system dedicated solely to the health and well-being of children, Children’s Wisconsin attracts some of the most pioneering researchers in their fields. When conventional methods don’t work, researchers at Children’s Wisconsin leap into the unknown, working collaboratively with academic partners at the Medical College of Wisconsin to translate innovative ideas into new medical breakthroughs.
“We review trials critically as a group and we open trials that we feel would potentially be beneficial for our patients. We feel very strongly the science has to be there,” said Dr. Talano. “When we’re in a situation where we’ve tried conventional treatments and it’s not working, it’s important to have the ability to offer these additional protocols for patients.”
The Children’s Wisconsin Research Institute, in partnership with the MACC Fund Research Center at the Medical College of Wisconsin, represent the most powerful concentration of pediatric research in southeastern Wisconsin. At any given time, doctors in the MACC Fund Center for Cancer and Blood Disorders are involved in upwards of 140 clinical trials. Research and innovation are key components of Children’s Wisconsin and that’s especially true when it comes to treatment for cancer and blood disorders.
“Clinical research is paramount to what we do in pediatric oncology and bone marrow transplant,” said Dr. Talano. “By performing clinical research, we are advancing the field with the goal of treating patients more successfully with fewer long-term side effects. Our commitment to clinical research and support from the MACC Fund organization has made this possible at our center. Without these partners we would not be as successful as we are.”
A return to normalcy
 So much of Yasmeen’s early life was spent at Children’s Wisconsin — many birthdays, Christmases, Halloweens were celebrated here, miles away from her home, her friends, her family. But in the 11 years since Yasmeen received that experimental treatment, her life has taken on a normalcy her parents once only dreamed of.
So much of Yasmeen’s early life was spent at Children’s Wisconsin — many birthdays, Christmases, Halloweens were celebrated here, miles away from her home, her friends, her family. But in the 11 years since Yasmeen received that experimental treatment, her life has taken on a normalcy her parents once only dreamed of.
But her story wasn’t over. For many years after her successful treatment, Yasmeen still came up to Children’s Wisconsin once a year to check in with the Survivorship Program — for kids with cancer, their journey doesn’t end with remissions. Life after cancer can often be difficult and uncertain, filled with follow-up care, potential long-term effects of treatment, maintaining a healthy lifestyle and the fear of recurrence.
Children’s Wisconsin established the Next Steps Survivorship Program in May 2001 and sees more than 200 cancer survivors every year. The program helps patients and families identify and monitor possible late effects, educates on ways to maintain a healthy lifestyle based on risk factors and empowers survivors to advocate for their health. Their goal is to help survivors live happy, healthy lives.
“They would review her blood work and lab results to make sure the cells weren’t coming back,” said Ivan.
“But it was very wide-ranging, encompassing every aspect of her life,” Judy added. “They were checking on not only her medical status but also school, her mental health, any emotional needs — just her overall wellness. It was very supportive.”
This level of care is only possible because of Children’s generous partners including the MACC Fund, Northwestern Mutual, and the Gold In September (G9) Program of Beat Childhood Cancer. Philanthropy powers everything from leading-edge treatments to child life services to the cancer survivorship program, allowing Children’s to provide the best and most seamless care to families like Yasmeen’s.
Yasmeen is now 17 years old. She’s a junior in high school and, thankfully, much of the pain and difficulties she endured as a child have faded into the past. She loves crafting, anime and hanging out with her friends — very much your typical teenage girl.
And after all she has gone through, typical is all she ever wanted.







