Monica Farr will never forget the first time she saw her son, Ma’Siah, turn blue.
He was just a newborn and as he struggled and gasped to breathe, Monica grabbed him and ran to her car, throwing her keys to her then 16-year-old daughter, Maliyah.
 As Maliyah raced them to the nearest emergency room, Monica sat with Ma’Siah in the backseat, praying they would make it to the hospital in time. The ER doctors at that hospital stabilized Ma’Siah and told Monica he was simply born with small airways and a floppy trachea.
As Maliyah raced them to the nearest emergency room, Monica sat with Ma’Siah in the backseat, praying they would make it to the hospital in time. The ER doctors at that hospital stabilized Ma’Siah and told Monica he was simply born with small airways and a floppy trachea.
But that wasn’t the last time they would rush to the hospital in fear of Ma’Siah’s life, and Monica quickly became her son’s biggest advocate. Monica would sit with her notepad and pen, ask questions and wonder what would happen if they didn’t get to the hospital in time.
After years of frustration at other hospitals, where Monica felt unheard and brushed off, she took Ma’Siah to Children’s Wisconsin. There, they met Joshua Steinberg, MD, a pediatric specialist in the Children’s Wisconsin Allergy, Asthma and Immunology Program.
Ma’Siah was 5 years old when Dr. Steinberg officially diagnosed him with asthma. Ma’Siah and Monica had gone through five years of believing it was small airways and a floppy trachea causing his breathing difficulties. Five years of rushing to the hospital, not knowing what else to do.
During one of those initial visits after the diagnosis, Monica, exhausted from not knowing how to properly address Ma’Siah’s breathing difficulties and how to prevent his asthma attacks, got emotional while asking Dr. Steinberg how she could help her son.
“There’s a program here at Children’s Wisconsin that I believe would be helpful to you and Ma’Siah,” said Dr. Steinberg. “I’m going to introduce you to the person who helps us run it.”
That person, Dorian James, would transform Ma’Siah and Monica’s lives.
A childhood epidemic
 Dorian was an asthma management program coordinator for Children’s Wisconsin. In that role, he helped run the Children’s Wisconsin Community Health Asthma Management Program (CHAMP), which addresses the inequities behind health risks, like asthma, in pediatric communities. Not just limited to treating the physical ailment, CHAMP gets a picture of a child’s whole health by assessing their home and social needs. The program acts as a community navigator of assistance across the aboard — relocation assistance, housing, food, transportation, utilities and other social needs. Every year, Dorian serves about a hundred families through CHAMP.
Dorian was an asthma management program coordinator for Children’s Wisconsin. In that role, he helped run the Children’s Wisconsin Community Health Asthma Management Program (CHAMP), which addresses the inequities behind health risks, like asthma, in pediatric communities. Not just limited to treating the physical ailment, CHAMP gets a picture of a child’s whole health by assessing their home and social needs. The program acts as a community navigator of assistance across the aboard — relocation assistance, housing, food, transportation, utilities and other social needs. Every year, Dorian serves about a hundred families through CHAMP.
In the United States, 1 in 12 kids age 0-17 — that’s about 6 million children — have asthma.
Asthma is a serious disease, causing wheezing, difficulty breathing and coughing. Over a lifetime, it can cause permanent lung damage. According to the Centers for Disease Control and Prevention (CDC), about 16 percent of Black children and 7 percent of white children have asthma. Every year, 1 in 6 children with asthma visits the emergency department with about 1 in 20 children hospitalized for asthma. Emergency department and urgent care center visits related to asthma attacks were highest among children ages 0-4 years old and non-Hispanic Black children.
Ma’Siah is one of these affected children.
The advocate every child deserves
 When Monica started getting the education from Dorian, she said it was baby steps. But the little things add up to a lot in changing your child’s health for the better.
When Monica started getting the education from Dorian, she said it was baby steps. But the little things add up to a lot in changing your child’s health for the better.
“There’s a saying, ‘strengthen your strengths and resource your weaknesses,’” said Monica. “Dorian was the resource in addressing Ma’Siah’s health challenges.”
Dorian and the CHAMP team visited Monica’s home to assess possible asthma triggers and then created a personalized plan. They ensured Ma’Siah receives needed services, and Monica was equipped with resources the home needs.
“The more I know and understand, the better I can help those who are suffering,” said Dorian. “Chronic conditions like asthma reside heavily in low-income populations, where children live in an environment where there might be extensive mold, roaches, rats, rat feces. A lot of their residences are in high-traffic areas, by freeways, by landfills or factories with smoke stacks, where there’s a lot of pollution going into the air they’re breathing.”
Dorian said even children who are not predisposed end up in the emergency room because they develop asthma from their unhealthy environment.
For those who do not have the genes, he said, the exposure to mites, to the propane, to all of the environmental triggers they live in, causes changes inside their lungs, sometimes irreparable. Studies show that up to 60 percent of health is determined by zip code rather than genetic code.
When Dorian went to Monica’s home, he discovered the vents needed to be cleaned out, and through a grant, he was also able to buy an air purifier for them.
Monica recalls a time when Ma’Siah had been stung by a bee at school. She called Dorian, panicking. Dorian was pulling up to their house just as the school bus was dropping Ma’Siah off, to let them both know Ma’Siah would be okay. When Ma’Siah caught COVID-19 last January, through the fever, through the breathing treatments, it was Dorian who helped calm her down.
“If I could wave a magic wand and create more Dorians, I would,” said Monica.
Dorian was the glue between the family and the doctor, the advocate for her child, the person who made time to answer all and any of her questions.
Thanks to Dorian’s guidance and intervention, today, Ma’Siah is the lovable, free-spirited 8-year-boy he deserves to be. He loves riding his bicycle, doing karate and playing games. He’s no longer afraid of being active or going outside, as he once was.
The price of asthma on children’s lives
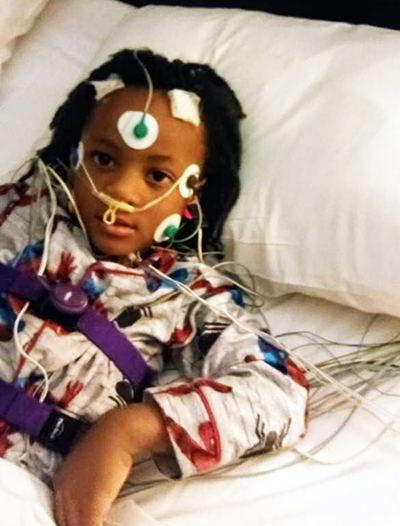 Asthma is the number one cause of absenteeism in schools in the country, and one of the top three diagnoses in the emergency room in the country.
Asthma is the number one cause of absenteeism in schools in the country, and one of the top three diagnoses in the emergency room in the country.
Dorian said the biggest challenge is the physical health, but a close second obstacle is the psychological component. What do kids want? They want to be liked and be friends with everyone. With asthma, exertion and exercise is a trigger for their asthma. The kids feel shame because they have to avoid exertion, they can’t overdo it in gym, they can’t get too mad or laugh too hard because it might trigger it. They can’t go outside with their friends and play, and they are sleep-deprived due to difficulties breathing at nighttime.
Those who are newly diagnosed, Dorian said, don’t realize what’s going on. Those who have grown up with asthma, he has observed, abnormal breathing is their baseline. One of the hardest parts he contends with is reaching the children and families who need the information the most.
“My job is ensuring the children get the health care attention they need, and educating the parents, making sure they appreciate the severity of this condition, providing resources to them to make the changes needed to make the environment better for the child and the entire family,” said Dorian. “Sometimes that means moving to new housing.”
He encourages families who believe their child has displayed symptoms to call their child’s pediatrician immediately. If a child has a bad asthma attack, the outcome carries the risk that the child may need breathing treatments, they may need to be intubated, and worst case scenario, they may not survive the asthma attack.
One size does not fit all
One of the other children he saw, Anthony, was 3 years old when he was first seen in Children’s Wisconsin Emergency Department. For years following, he had multiple inpatient admissions due to his acute symptoms.
After one inpatient visit, he was referred to Children’s Wisconsin Asthma, Allergy and Immunology Program. However, there were barriers that made it difficult for the family to follow through. Anthony missed a number of appointments, was not always taking his medication as prescribed, and continued to need emergency and inpatient care.
In Anthony’s case, one size did not fit all. The standard of care was not providing what the family needed to ensure an equitable outcome. A few years later, Children’s Wisconsin case management team referred Anthony, who was then 9 years old, to CHAMP.
Dorian visited Anthony’s home and established a trusted relationship with the family. By providing care for them where they live and work, he was able to reduce barriers of access.
He provided education and served as a liaison to other members of Anthony’s care team, including communicating with the Asthma, Allergy and Immunology team about Anthony’s progress. During his visits, Dorian became aware that there was mold in the home, which can be a serious asthma trigger.
Since Anthony’s health insurance was provided by Chorus Community Health Plans (CCHP – formerly Children's Community Health Plan), Dorian referred the family to the plan’s housing program. A housing navigator from CCHP assessed the family’s situation and worked with them to find a new home that did not have asthma triggers present.
In the years since Dorian established a relationship with Anthony and his family and provided the extended care services, Anthony’s asthma has improved and he has not needed any further emergency or inpatient care. However, the work is not done. After a few months, the family missed a few appointments with the Asthma, Allergy and Immunology Program, requiring Dorian to reach out again to assess any further needs they have and help remove additional obstacles to Anthony’s care.
By working together on these children’s behalf, Children’s Wisconsin and the CHAMP team are vital for children and families in Wisconsin. Children’s Wisconsin is working to better implement connections with kids and families, and provide coordinated and holistic care that ensures equity throughout our health system.
Signs and symptoms of asthma
If you believe your child may have one of the symptoms below, please make an appointment online or call (877) 607-5280.
- A cough, can be constant, or comes and goes
- Wheezing or whistling sound heard while the child is breathing
- Trouble breathing or shortness of breath while the child is active
- Chest tightness
- Tiredness
- Cough at night
- Noisy breathing







