It was around noon on Dec. 17, 2021. Beyonca Jones was home cleaning when she got a call from Whitman Middle School in Wauwatosa. Her 13-year-old daughter, Yejah, wasn’t feeling well, so Beyonca picked her up early and brought her home.
At first, it was just a cough, but over the course of the day, Yejah also developed a fever and headache. By the next day, she was having a hard time breathing.
“She said it felt like someone was standing on her chest,” said Beyonca.
A quick trip to the Children’s Wisconsin Emergency Department (ED) confirmed what everyone suspected: Yejah had COVID-19. She was quickly admitted to the hospital.
Two days later, Yejah’s older sister, 17-year-old Shaunye, also developed a cough and headache. And just like Yejah, the next day she started having difficulty breathing. Another trip to the Children’s Wisconsin ED and another positive COVID-19 test soon followed, and Shaunye joined her sister in the hospital.
Throughout the COVID-19 pandemic, there has been one constant — kids tend to experience much milder symptoms than adults. So, by and large, kids requiring hospitalization due to COVID-19 are rare. But despite that, and despite the fact that Yejah and Shaunye were both vaccinated, the treatment they received wasn’t the standard protocol for a child with COVID-19.
In a standard case of COVID-19 in a child with no underlying health issues, the child would typically be instructed to quarantine at home, push fluids and take over-the-counter medications to manage the symptoms until their body’s immune system cleared the infection.
But Yejah and Shaunye were admitted to Children’s Wisconsin and received monoclonal antibodies — a more intense treatment regimen that can interfere with how the COVID-19 virus infects cells — because they have an underlying health condition that put them at greater risk for severe symptoms. Both sisters have sickle cell disease.
What is sickle cell disease?
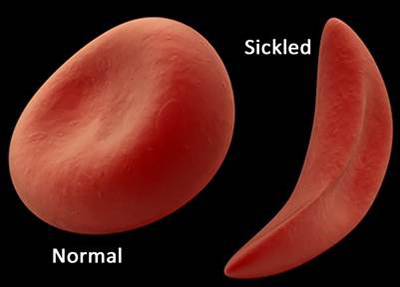 Sickle cell disease is a chronic condition that affects hemoglobin, the protein in red blood cells, and causes a person’s red blood cells to be misshapen. Instead of smooth, round and flexible, the cells are stiff and shaped like a crescent. When this happens, the cells can get clogged as they travel through veins and arteries, which can lead to complications such as extreme pain, severe lung problems or strokes. Additionally, sickle cells only live for about 15 days, as opposed to up to 120 days for healthy cells. As a result, people with sickle disease also suffer from severe anemia, a decrease in red blood cells in the body.
Sickle cell disease is a chronic condition that affects hemoglobin, the protein in red blood cells, and causes a person’s red blood cells to be misshapen. Instead of smooth, round and flexible, the cells are stiff and shaped like a crescent. When this happens, the cells can get clogged as they travel through veins and arteries, which can lead to complications such as extreme pain, severe lung problems or strokes. Additionally, sickle cells only live for about 15 days, as opposed to up to 120 days for healthy cells. As a result, people with sickle disease also suffer from severe anemia, a decrease in red blood cells in the body.
In the United States, approximately 100,000 people have sickle cell disease, the vast majority of whom are Black. Sickle cell disease actually developed as an evolutionary defense against malaria, so it affects people who are decedents from parts of the world where malaria is prevalent, such as sub-Saharan Africa, South and Central America, Saudi Arabia, India and the Mediterranean.
In the beginning of 2020, doctors all over the world were working tirelessly to learn as much as possible about COVID-19. While their main focus was how to stop it, another key area of research was how it interacted with other chronic diseases.
“We had reason to believe that because of sickle cell complications, COVID-19 would be worse in those patients, but we didn’t know for sure,” said Amanda Brandow, DO, MS, pediatric hematologist-oncologist at Children’s Wisconsin. “We had a clinical need to see how COVID-19 affected kids with sickle cell.”
Gathering data and learning rapidly
At Children’s Wisconsin, the MACC Fund Center for Cancer and Blood Disorders has one of the region’s largest Sickle Cell Disease Clinics, treating as many as 380 kids a year. Combined with the MACC Fund Research Center at the Medical College of Wisconsin, the academic partner of Children’s Wisconsin, Dr. Brandow and her team were uniquely qualified to investigate the impact COVID-19 might have on people living with sickle cell disease.
On March 20, 2020, shortly after COVID-19 was detected in the United States, Dr. Brandow along with her former colleague Julie Panepinto, MD, set up a SECURE-SCD Registry to track people with sickle cell disease who contracted COVID-19. The registry included demographic data on the patient, how severe their symptoms were, what the outcome of their disease was and any other health conditions they may have. The registry was open to institutions all over the world and the number of cases added quickly grew to more than 900.
“We needed to learn rapidly and the real-time reporting registry allowed us early on to learn what the effects of COVID-19 were on kids with sickle cell disease,” said Dr. Brandow, who is also a professor of pediatrics in the section of hematology/oncology/bone marrow transplantation at The Medical College of Wisconsin. “We compared the characteristics of individuals with sickle cell disease who had serious COVID-19 illness to individuals with sickle cell disease who had mild COVID-19 illness.”
Thanks to the registry, Dr. Brandow and her team learned kids with sickle cell disease were at higher risk for severe cases of COVID-19 illness. Further, they also learned what aspects of sickle cell disease increased a person’s risk for having worse COVID-19 illness. “We found that kids with sickle cell disease who had previous pain episodes or prior heart, lung or kidney problems were at higher risk for more serious COVID-19 illness, hospitalization, and development of a new pain episode during their COVID-19 infection,” said Dr. Brandow.
In late April, the Centers for Disease Control and Prevention (CDC) learned of the registry and connected with Dr. Brandow and her team about their findings.
“When the CDC found out about our registry, they approached us to learn more about it and to ask if they could collaborate with us on a publication from the data,” said Dr. Brandow. “We published an initial analysis of our data with the CDC in the journal Emerging Infectious Diseases in July 2020.”
In October 2020, the CDC added sickle cell disease to their list of medical conditions that put people at increased risk of severe COVID-19. Because of that designation, thousands of people with sickle cell disease — like Yejah and Shaunye — were able to receive more intense treatment when they contracted COVID-19 and were given priority access to the vaccine when it was first made available.
“Our data directly informed the CDC recommendation to designate sickle cell disease as a high-risk condition for COVID-19 early on in the pandemic,” said Dr. Brandow.
For Yejah and Shaunye, thanks to the enhanced treatment, their symptoms never got too serious. Neither girl needed to be put on a ventilator and both were able to go home on Dec. 24. But were it not for the quick action and thorough research of Dr. Brandow and her MACC Fund Center and Medical College colleagues, there’s no telling how much more serious their cases may have been.







