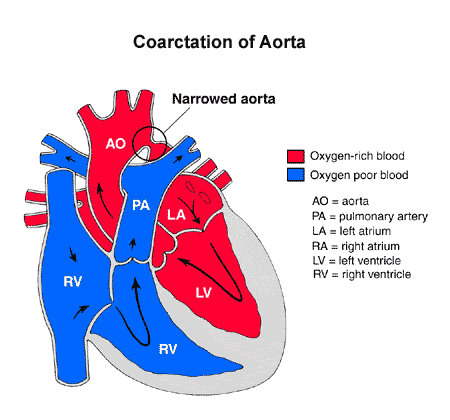
Coarctation of the aorta is a condition that someone is born with (congenital). It happens when the fetal heart doesn’t develop normally during the first two months of pregnancy. This occurs when there is abnormal development of the aorta before birth. The aorta is the large artery that carries oxygen-rich (red) blood to the body. In coarctation, it is narrower than it should be, making it harder for the heart (left ventricle) to pump blood past the narrowing. Depending on the amount of narrowing, it can present at different ages from newborn to adults.
Coarctation of the aorta can cause several problems, including:
- The left ventricle that pumps blood to the body cannot squeeze/pump well due to overwork.
- Blood pressure is higher above the narrowing (right arm) and lower below the narrowing (leg).
- In severe narrowing, it can be hard for the organs in the abdomen (kidneys, liver, intestines) to get enough blood flow and it can cause organ failure or feeding problems in the newborn.
- High pressure can weaken the walls of the heart. That can lead to uncontrollable bleeding or stroke.
- There is an increased risk of developing an infection of the valves of the heart or aorta. This is called bacterial endocarditis.
- The coronary arteries, which supply oxygen-rich (red) blood to the heart muscle, may narrow in response to long-standing elevated pressure.

