March 15, 2021. It was an unseasonably warm, early spring day and Cara Bonnell was at Silver Spring Intermediate School where she teaches special education to fifth and sixth graders. As Cara was walking with a student through the cafeteria — the far wall of windows filled with a sheet of overcast gray — a sudden wave of dizziness engulfed her.
In the fog, Cara took a few uneasy steps before reaching out and bracing herself against one of the round, wooden tables to keep from falling over. She stumbled about 10 more steps to another table along the back wall, where she finally sat down to collect herself. Beads of cold sweat collected on her forehead. After a couple minutes, Cara got back to her feet and was able to slowly get herself to the nurse’s office.
The school nurse took her temperature and it was really low. Somewhere around 95 or 96 degrees, Cara vaguely recalled. The nurse suggested they call an ambulance, but Cara resisted, not wanting to make a big deal out of it. After about 15 minutes, the dizziness didn’t get any better, so they called her emergency contact, her mother, who came and picked her up. They were going to drive to the nearest emergency department.
“They had to take me out in a wheelchair,” Cara remembers. “I couldn't even function.”
In the emergency department, Cara was immediately taken back to a room and a medical assistant started taking her vitals. The assistant took her temperature and then started to strap the blood pressure cuff onto Cara’s arm.
On Cara’s left wrist is a blue Apple Watch strap that is also her medical ID bracelet. It reads:
CARA BONNELL
COARC S/P REPAIR
A0 ANEUYRSM S/P REPAIR
ABSENT PULSE BIL ARMS
BP LEFT LEG ONLY
A heart built differently
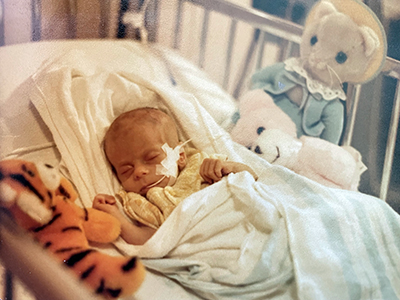
The aorta is the main artery that branches off from the top of the heart and delivers oxygen-rich blood throughout the body. When Cara was born, her aorta had multiple congenital defects. It was narrower than normal (coarctation of the aorta), it had an opening in it to the other major artery of the heart (patent ductus arteriosus) and the main valve was malformed (bicuspid aortic valve). She also had a ventricular septal defect, which is a hole in the wall that separates the two lower chambers of the heart. Combined, the defects prevented her heart from effectively pumping blood.
When she was about 1 week old, Cara had an open-heart surgery to repair the defects. She would need another surgery when she was 2. While in college, she needed a third surgery after her aorta developed a bulge, a serious condition known as an aortic root aneurysm. As a result of these defects and the multiple corrective surgeries, Cara’s anatomy doesn’t always look and function as one might expect — not even to a trained medical professional. Which brings us back to that day in the emergency department.
“I thought, you can’t take my blood pressure from my arm, it’s not accurate,” said Cara. “But at that point, I was just like, whatever, they're the experts. It said my blood pressure was fine. Around 130.”
After a couple hours in the emergency department, the doctors told Cara she was just a little bit dehydrated and had vertigo. They sent her home and told her to follow-up with her primary care doctor if she didn’t feel better in a day or two.
As the days went on, Cara continued to have episodes where she felt like she was going to pass out, so she made an appointment with her primary care doctor. Again, she encountered the same issues with measuring her blood pressure.
"Before I saw my doctor, the medical assistant came in and said she was going to take my blood pressure,” said Cara. “I told her, ‘You have to take it in my leg. It's not accurate in my arms.’ And I'll never forget what she said. She said, ‘Oh honey, we don't care what your blood pressure is. We only care if it's different from when you're laying down to standing up.’ They still thought it was vertigo.”
Again, the blood pressure reading from her arm was fine. The doctor told her she likely had a little fluid in her ear that caused the vertigo and he gave her some nasal spray. He advised her if it didn’t get better after a few days, to follow up with an ear, nose and throat specialist.
A new frontier in health care
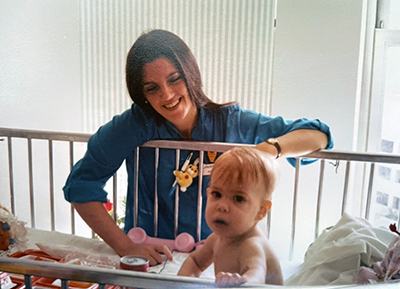 Cara was born in 1979, which in terms of medical care — especially congenital heart disease care — might as well be 1,000 years ago. Prior to about 1944, most children born with congenital heart defects didn’t survive. Even as recently as the late 1980s, about 25 percent of children born with severe heart defects died before their 1st birthday.
Cara was born in 1979, which in terms of medical care — especially congenital heart disease care — might as well be 1,000 years ago. Prior to about 1944, most children born with congenital heart defects didn’t survive. Even as recently as the late 1980s, about 25 percent of children born with severe heart defects died before their 1st birthday.
Today, that figure is less than 5 percent.
That means, today, people born with congenital heart defects are now living well into adulthood. In fact, in the United States, there are as many as 1.4 million adults living with congenital heart disease. It’s a remarkable story of medical advancement. However, these men and women require lifelong, specialized medical care and management. And they pose a unique challenge for doctors.
Adult cardiologists are great at treating heart disease acquired by age or lifestyle factors. But that’s very different than a heart defect that’s present at birth. At the same time, pediatric cardiologists, by definition, aren’t trained to care for the needs of an adult. So, as a child with a heart defect grows into adulthood, they enter into a health care no man’s land.
That’s why in 2004, Children’s Wisconsin started the Adult Congenital Heart Disease Program. This was the first program in Wisconsin and one of the first in the nation to be dedicated exclusively to the care of adults who were born with heart defects.
“It’s a unique niche in the field of cardiology,” Salil Ginde, MD, Cara’s cardiologist at the Herma Heart Institute at Children’s Wisconsin. “We have all these patients that are surviving to adulthood, but 15 years ago, there was no consistent medical home for them.”
From one doctor following a hundred patients in 2004, to five doctors today who are board-certified in Adult Congenital Heart Disease and care for more than 2,700 patients a year. With seven outreach sites located throughout Wisconsin and upper Michigan, the program is the largest in the state.
The third time…
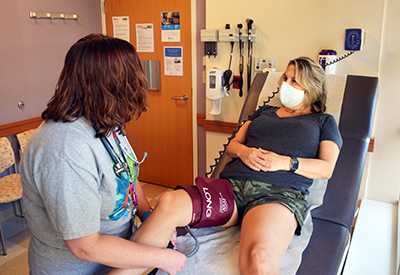 Weeks after they started, Cara’s dizzy spells persisted. So, per her doctor’s orders, Cara scheduled an appointment with an ear, nose and throat (ENT) specialist. And again, the nurse came in to take her blood pressure.
Weeks after they started, Cara’s dizzy spells persisted. So, per her doctor’s orders, Cara scheduled an appointment with an ear, nose and throat (ENT) specialist. And again, the nurse came in to take her blood pressure.
“I said, ‘Listen, you have to take it in my leg.’ And the woman goes, ‘I don't even know how.’”
Cara decided to take matters into her own hands. She took the blood pressure cuff from the nurse and slid it up her left leg right below the knee, then cinched the Velcro down tight.
“I don't remember what the bottom number was,” said Cara, “but the top number was 212.”
Finally, for the first time after three doctors' visits, the ENT specialist raised the possibility of Cara’s heart as the underlying cause for her dizzy spells. Cara recalls him saying that he didn’t doubt she might have a little bit of vertigo, but a lot of times what people think is related to ENT is actually caused by blood pressure. He insisted she see her cardiologist. Cara texted her sister, Emily, who is also a nurse at the Herma Heart Institute at Children’s Wisconsin.
“She said, ‘Come here right now,’” Cara said. “I left the ENT and went right to the Herma Heart Institute.”
Not only is Dr. Ginde a pediatric cardiologist, he is also board certified in adult congenital heart disease, meaning he understands the unique nature of heart defects that regular adult cardiologists often don’t. After a series of tests and reviewing her complex medical history, Dr. Ginde determined that Cara’s aorta had narrowed again, significantly. As a result, her blood pressure, especially in her brain, was getting dangerously high.
“It was a very unusual presentation of symptoms. Lightheadedness can be common, but vertigo with the room spinning is very different. I don’t think the other physicians did anything wrong. Given the presentation, it made sense to look at other issues,” said Dr. Ginde. “But it was fairly serious. The vertigo she was experiencing was because she wasn’t getting enough blood flow to the brain. She was having early signs of a stroke.”
On April 15, a month after the dizziness started and 15 years since her previous one, Cara went in for a heart catheterization. In this three-hour long procedure, Dan McLennan, MD, an interventional cardiologist, threaded a small metal wire into an artery in Cara’s groin and fed it up to the aorta. He then inflated a tiny balloon in order to stretch the aorta out and increase the blood flow.
Because of Cara’s previous surgeries and procedures, the catheterization was high-risk. During her third surgery in college, Cara had a stent placed in her aorta, a tube of wire mesh to keep the artery open. The chance of that stent rupturing during this procedure and causing life-threatening internal bleeding was very high. And, in fact, that’s exactly what happened. Thankfully, due to Dr. McLennan’s experience treating adults with congenital heart disease, he planned for the complication and was able to identify and treat it immediately.
“His understanding of her complex anatomy was critical. If he didn’t recognize it as fast as he did, just a couple more minutes, and her heart would have stopped,” said Dr. Ginde. “It was remarkable. He was really prepared and we had the proper equipment and technologies ready, which aren’t readily available in an adult cath lab.”
Cara spent a few days recovering, but almost immediately, oxygen-rich blood began to once again course through her body and her dizziness went away.
Advocate for yourself
 Cara first came to the Herma Heart Institute’s Adult Congenital Heart Disease Program in 2009, after she moved to Milwaukee from central Illinois. Prior to coming to Milwaukee, Cara moved around a lot and didn’t have a consistent cardiologist.
Cara first came to the Herma Heart Institute’s Adult Congenital Heart Disease Program in 2009, after she moved to Milwaukee from central Illinois. Prior to coming to Milwaukee, Cara moved around a lot and didn’t have a consistent cardiologist.
“I definitely had some lapse in care in my early 20s,” said Cara.
That’s, unfortunately, all too common for young adults, but it’s not a safe option for individuals living with congenital heart disease. And it speaks to the need not only for specially trained adult congenital heart disease doctors, but also for patients to advocate for themselves in adult health care settings where staff may not be familiar with congenital heart defects.
“These patients are very complicated with unique anatomy,” said Dr. Ginde. “Unless you have specialized training in congenital heart disease, it’s very difficult to recognize atypical symptoms and know how to treat them.”
“Kids who were born with heart defects, we're adults now. And a lot of adult providers just don't know,” said Cara. “That’s why I love the Adult Congenital Heart Disease Program at the Herma Heart Institute, they know their stuff. They’re really knowledgeable and on the forefront of knowing what to do. It's just a really great program. I feel really taken care of there.”
Though Cara had been keeping up with her annual cardiac follow-up appointments, this recent scare taught her an important lesson about the need to speak up for yourself and your health needs. And she hopes others like her will follow suit.
“People know their bodies best. You really can't be afraid to open your mouth and advocate for yourself,” said Cara. “It's your health. It's your body.”







