The providers at Children’s Wisconsin work tirelessly to save kids’ lives every single day. They treat pediatric cancer, perform life-saving organ transplants, and remedy severe respiratory infections.
“We’re trained to believe we can make a difference,” said Steve Kindel, MD, pediatric cardiologist with the Herma Heart Institute at Children’s Wisconsin.
And the vast majority of the time, they can, and they do.
Except sometimes, they can’t. And it’s devastating. They feel grief to the very core of their soul, and often that grief is unseen and underappreciated.
 “You see and talk to these families every day,” said Dr. Kindel. “They’re going through the worst time of their lives. Many of us are parents ourselves, so when we can’t save their child, we all take it really hard. Logan was a particularly challenging case. He was healthy, until he wasn’t.”
“You see and talk to these families every day,” said Dr. Kindel. “They’re going through the worst time of their lives. Many of us are parents ourselves, so when we can’t save their child, we all take it really hard. Logan was a particularly challenging case. He was healthy, until he wasn’t.”
Logan Johnson was an 8-year-old boy. One Saturday morning in 2017, he was playing soccer. That night, he collapsed at home. His parents, Chris and Laurie, who are both nurses, waited anxiously for an ambulance to rush him to Children’s Wisconsin Milwaukee Hospital.
How did Logan get so sick?
His main complaint was abdominal pain, so providers did an exhaustive workup focused on his abdomen. It would be hours of extensive tests, ultrasounds and lab work before they had their answer.
An abdominal CT scan happened to catch fluid around Logan’s heart. An astute surgical fellow then decided to do a bedside point of care ultrasound (POCUS) on Logan’s heart — a procedure that wasn’t routine at the time. He noticed his heart was weak, not squeezing well, and depriving the rest of his organs from getting enough blood. The Cardiac Intensive Care Unit (CICU) team quickly moved to do a complete echocardiogram, a formal cardiac ultrasound. They promptly determined Logan was suffering from acute myocarditis — inflammation of the heart typically caused by a viral infection that dramatically affects organ function.
As the doctors and surgeons worked to save Logan, he suffered a cardiac arrest and a severe neurologic injury. After three weeks on life support with no recovery of his heart or brain functions, Logan’s family made the excruciating decision to withdraw support. Logan passed away on May 27, 2017.
Remembering Logan
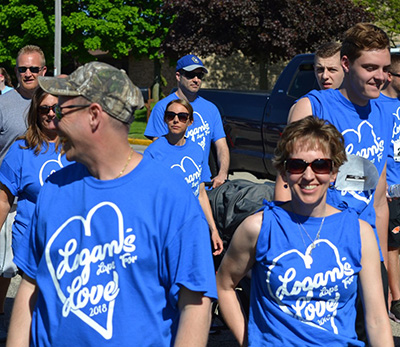 Following Logan’s death, his family knew immediately they wanted to channel their grief, and the grief of their community, into something positive. And, they wanted to find a way to support the doctors and nurses who had fought so hard to save Logan.
Following Logan’s death, his family knew immediately they wanted to channel their grief, and the grief of their community, into something positive. And, they wanted to find a way to support the doctors and nurses who had fought so hard to save Logan.
“I wanted people to remember Logan and say his name every year,” said Laurie.
The Johnson family started Logan's Laps for Love, an annual fundraising event. They also established the Love for Logan fund through the Children’s Wisconsin Foundation to raise awareness of myocarditis and help kids achieve an earlier diagnosis.
“Logan had no signs that showed how bad his heart was,” said Laurie. “There wasn’t quite enough evidence to point to one thing. Our goal became finding a way to get kids from the Emergency Department to the CICU quicker. We wanted to connect the dots faster so that another child could get a more immediate diagnosis.”
In addition to grieving and fundraising, Laurie and Chris personally began working with doctors at Children’s Wisconsin to develop a list of signs and symptoms that would indicate a child might be experiencing myocarditis. “When a child comes into the Emergency Department with varied symptoms, it may not be immediately clear that they have a heart issue,” said Patrick Drayna, MD, a pediatric emergency medicine physician at Children’s Wisconsin. “It becomes more about a screening process, ruling in and ruling out. The Johnson family supported the development of a decision tree of clinical criteria that points to the heart so we can more quickly make a diagnosis.”
The result is “Logan’s Protocol,” a guideline for early detection and management of myocarditis and other illnesses of the heart. The protocol includes labs, a chest x-ray, an EKG and a point of care ultrasound.
“What ultimately made the difference for Logan was the point of care ultrasound,” said Laurie. “Once the ultrasound showed his heart, we had a diagnosis within minutes.”
The use of POCUS in pediatric emergency departments has been limited due to a lack of funding for training. National accreditation is $4,000 per person. Jake Scott, MD, a pediatric anesthesiologist and critical care physician at Children’s Wisconsin, and Dr. Drayna, lead the POCUS initiative in the Pediatric Intensive Care Unit (PICU) and Emergency Department (ED), respectively. They are responsible for teaching the utility of POCUS and identifying providers for training.
Each year, the Love for Logan fund supports 2-5 providers in the ED and PICU to be trained in POCUS to scan for organ dysfunction right at the bedside. Recently, Children’s Wisconsin expanded the training to include advanced practice nurses and senior fellows.
To reach Laurie’s goal of making Logan’s Protocol universal, it will need to go outside of Children’s Wisconsin and become part of the national conversation. Dr. Scott and Dr. Drayna believe it will become a standard of care in pediatric institutions within 5-10 years, but it will require data, awareness, outreach and time.
In addition to being physicians, Dr. Scott, Dr. Drayna and Dr. Kindel are also faculty at the Medical College of Wisconsin — the academic partner of Children’s Wisconsin. It’s this commitment and connection to academic medicine that empowers these providers to continuously learn and innovate. As a result, their healing impact stretches far beyond the walls of Children’s Wisconsin.
Unexpected healing
 While the Johnson family’s advocacy is a light carrying them through darkness, the providers didn’t realize how much the journey with this family, along with the Love for Logan fund and resulting collaboration, would help them heal.
While the Johnson family’s advocacy is a light carrying them through darkness, the providers didn’t realize how much the journey with this family, along with the Love for Logan fund and resulting collaboration, would help them heal.
“Logan’s story is reflective of other stories where we don’t always have the outcome we want, try as we might, to the best of our abilities,” said Dr. Drayna. “Sometimes it feels like you’re trying to hold on to a handful of sand and reaching for the tools you have at the time. That can be frustrating and disheartening because you want to help and it’s hard when you can’t. To see how a bad situation can ultimately be turned into a source of strength is uplifting and helps us move on.”
Maryanne Kessel, RN, is executive director and health system liaison for the Children’s Wisconsin Foundation. She has worked with the Johnson family since Logan’s death to create a path for the family’s continued connection with Logan’s clinical care team. She also helped them establish their foundation and now the Love for Logan general use fund at Children’s Wisconsin.
“Sometimes doctors get overlooked, as if they’re made of steel,” said Maryanne. “People expect them to pull their brains out and share something brilliant but forget that they’re people, too. Often, we speak of ‘wrapping our arms around our families’ during difficult times. Logan’s story is a powerful example of the Johnson family turning around and caring for our providers right back.”
For Dr. Kindel, the Johnson family’s energy and commitment inspired him and helped him focus on a new goal.
“Most families don’t want to sit in the memory of the worst possible thing that they’ve gone through,” said Dr. Kindel. “But some families go the other way and lean into it so they can put meaning to their child’s death while honoring and remembering them. I find that amazing. The Johnsons are so positive and dedicated that they push me to try harder, be more creative and think of ways to do more.”
Logan’s Protocol and POCUS has resulted in multiples cases of early detection of myocarditis and other heart issues at Children’s Wisconsin that providers consider “saves.”
“We’re very grateful to the Johnson family because they’ve chosen to try to make things better and that’s helped us save other kids,” said Dr. Scott. “None of us will ever feel better about what happened to Logan, but knowing that we prevented it from happening again and that we’re supporting the Johnson family’s mission helps us recover.”
For Maryanne, it has been incredible to witness the gratitude cycle that’s occurred between the Johnson family and the doctors.
“The process of putting together Logan’s Laps for Love is healing for the Johnson family because they’re able to bring something tangible back to the people who tried to save their son’s life and help them have a more positive outcome,” said Maryanne. “And when our providers are able to make diagnoses faster and better with the money raised from the Johnson family, it’s healing for the providers. Together, they’ve turned a tragedy into something positive.”







