On the morning of July 9, 2021, Oneida Perez Leon awoke in her hospital room with a neonatologist standing at her bedside. The doctor told her that a transport team was on its way from Milwaukee to bring her newborn to Children’s Wisconsin.
Oneida had just given birth to a baby boy. She and her husband named him Luis. It had been a difficult delivery. She experienced contractions for two days prior to her scheduled induction. She was exhausted and didn’t understand what the doctor was telling her.
“I gave birth at 6 a.m.,” said Oneida. “The next morning, at 4 a.m., I still hadn’t slept and the nurse offered to take Luis to bathe him and do his SHINE test so I could get some rest.”
SHINE (Screening Hearts In NEwborns) is a tool used to identify serious heart problems that babies may have at birth. Providers use a pulse oximeter to check the oxygen level of the baby’s blood.
But baby Luis never came back to the room. Luis had a heart defect that had gone undetected during pregnancy.
“The doctor kept repeating it to my husband and me because we didn’t react,” said Oneida. “We were in shock. We didn’t understand how this could be true because he had seemed perfectly fine!”
A surprise diagnosis
 A few weeks earlier, a routine exam showed Oneida’s unborn baby had only gained 7 ounces in the previous month. Oneida’s doctor thought the baby might be suffering from an asymmetrical growth restriction — a condition where a fetus directs most of its energy to maintaining growth of vital organs, such as the brain and heart, at the expense of the liver, muscle and fat. So when baby Luis was born on July 8 weighing a healthy 8 pounds 7 ounces, Oneida and her husband, also named Luis, breathed a sigh of relief.
A few weeks earlier, a routine exam showed Oneida’s unborn baby had only gained 7 ounces in the previous month. Oneida’s doctor thought the baby might be suffering from an asymmetrical growth restriction — a condition where a fetus directs most of its energy to maintaining growth of vital organs, such as the brain and heart, at the expense of the liver, muscle and fat. So when baby Luis was born on July 8 weighing a healthy 8 pounds 7 ounces, Oneida and her husband, also named Luis, breathed a sigh of relief.
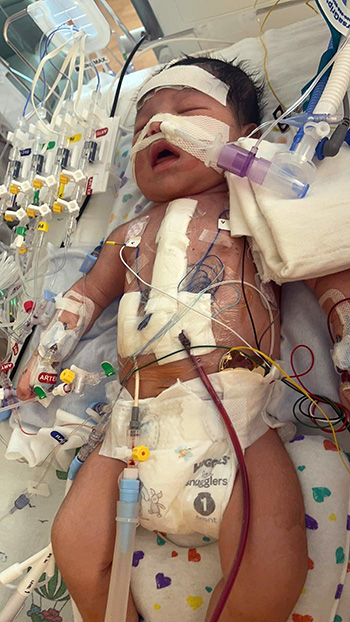
But the SHINE test revealed that Luis’ oxygen saturation level was low. His skin had also taken on a bluish tint because his blood wasn’t carrying enough oxygen. The neonatologist explained that Luis had tetralogy of Fallot, a serious grouping of four heart defects, including:
- Ventricular septal defect: A hole in the wall (septum) between the lower chambers — or ventricles — of the heart.
- Pulmonary stenosis: A narrowed or completely blocked pulmonary valve, which restricts blood flow from the heart to the lungs.
- Malposition of the aorta: The aorta is located directly above the ventricular septal defect, which is different from a normal heart where the aorta is completely on the left side. In addition, the aortic valve is enlarged and seems to open from both ventricles, rather than from the left ventricle only.
- Right ventricular hypertrophy: The muscular wall of the lower right chamber of the heart (right ventricle) is thicker than normal due to the narrowed pulmonary valve.
These defects affect the structure of the heart and cause oxygen-poor blood to flow out of the heart and to the rest of the body.
Luis actually had the most severe type of tetralogy of Fallot in which the pulmonary valve wasn’t just narrowed, but it didn’t form at all (pulmonary atresia). This is considered a critical congenital heart defect — one that requires surgery shortly after birth.
At just 5 days old, Baby Luis underwent open-heart surgery at Children’s Wisconsin. Ronald Woods, MD, PhD, a cardiothoracic surgeon at the Herma Heart Institute at Children’s Wisconsin, repaired the hole between the bottom chambers of Luis’ heart and placed a patch across the narrowed pulmonary valve to enlarge the passage to the pulmonary artery.
While the surgery was “nerve-wracking” for mom and dad, Luis did well and was able to go home about three weeks later.
A team effort
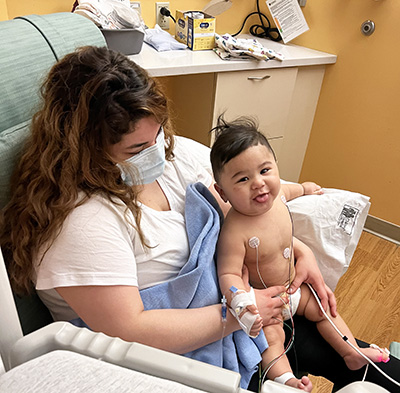 Kids with congenital heart defects need regular visits with a cardiologist for their entire lives to monitor their heart. In addition, most babies born with tetralogy of Fallot will need another procedure later in life, whether that’s an additional surgery or an intervention performed in a cardiac catheterization lab.
Kids with congenital heart defects need regular visits with a cardiologist for their entire lives to monitor their heart. In addition, most babies born with tetralogy of Fallot will need another procedure later in life, whether that’s an additional surgery or an intervention performed in a cardiac catheterization lab.
Luis began routine visits with Sara Creighton, MD, a pediatric cardiologist with the Herma Heart Institute who sees patients at Children’s Wisconsin hospitals in Milwaukee and Neenah. During Luis’ six-month follow-up visit with Dr. Creighton, an ultrasound showed that Luis once again had severely restricted blood flow to his lungs, which was also causing high pressure in his right ventricle.
“Sometimes things just don’t grow like we hope they will and there was a re-narrowing of Luis’ right ventricular outflow,” said Dr. Creighton. “Since Luis was less than a year out of surgery, I was hoping we could buy some time with an intervention that would avoid another open-heart surgery.”
Dr. Creighton got in touch with her interventional colleagues — cardiologists who do procedures in the cardiac catheterization lab as opposed to surgeons — to discuss Luis’ case.
During a catheterization, cardiologists insert long, flexible tubes (catheters) into a vein and/or artery of the legs, arms or neck. They then guide the catheters into the heart or surrounding blood vessels using X-rays to help guide them. Catheterization procedures are minimally invasive and help patients avoid surgery. Patients also benefit from less anesthesia time, less pain, faster recovery and shorter hospital stays.
The Herma Heart Institute at Children’s Wisconsin is one of the few pediatric heart institutes in the Midwest to have two state-of-the-art hybrid catheterization labs (operating room-caliber imaging suites) and three pediatric specialized catheterization doctors. Access to the cath labs gives Children’s Wisconsin cardiologists the flexibility to plan complex or multiple combined catheter and surgical procedures for a patient in the same procedure, if they feel it is best course of treatment. Children's Wisconsin offers all cardiac catheterization options for successfully diagnosing and treating pediatric and adult patients with complex congenital heart conditions.
Daniel McLennan, MD, a pediatric cardiologist with the Herma Heart Institute at Children’s Wisconsin who specializes in catheterization procedures, suggested to Dr. Creighton that Luis would be a great candidate for a cutting-edge procedure that would require special Food & Drug Administration (FDA) approval — a naturally absorbing stent.
A "divine" solution
 A stent is a piece of medical equipment that works to keep a narrow space open. Typically, stents are made of bare metal and are a fixed size — they don’t grow with the child. Most kids who need a stent will need a bigger one every couple of years as they grow, which means additional procedures. Plus, an outgrown stent needs to be surgically removed.
A stent is a piece of medical equipment that works to keep a narrow space open. Typically, stents are made of bare metal and are a fixed size — they don’t grow with the child. Most kids who need a stent will need a bigger one every couple of years as they grow, which means additional procedures. Plus, an outgrown stent needs to be surgically removed.
Dr. McLennan, however, was working with Lifetech, a leading developer and manufacturer of advanced minimally invasive medical devices for cardiovascular diseases and disorders, to create the first-ever naturally absorbing stent for children.
“Once you put in a bare metal stent, you’re committing the child to have a stent for life. But with a bioresorbable stent, you’re not,” said Dr. McLennan. “A bioresorbable stent takes 2-3 years to absorb, so as the child grows, the vessel has time to remodel itself and hopefully continue to grow normally and stay open.”
Dr. McLennan worked with Lifetech to make the bioresorbable stents of pure iron, a naturally occurring element in the body, which reduces the body’s inflammatory response that can sometimes cause re-narrowing. The result became Lifetech’s Iron Based Bioresorbable (IBS) “angel” stent.
“Dr. McLennan said the angel stent was still in the testing phase but it sounded like a perfect solution for Luis because it would improve his obstruction now without creating another problem to fix later,” said Dr. Creighton.
Parents Oneida and Luis were cautiously optimistic about the brand-new intervention.
“Anything is scary when it hasn’t been done a lot, but Dr. McLennan told us that if a regular stent collapsed, or when he needed a new one, they would have to go in and surgically remove the old one,” said Oneida. “All we were thinking is that we don’t want him to go through another surgery. We were willing to take the chance to avoid additional procedures.”
Children’s Wisconsin applied for and received emergency approval of the device from the FDA and the Institutional Review Board (IRB). Dr. McLennan and the Herma Heart Institute cardiac catheterization team placed Luis’ angel stent through a vein in his leg on March 24, 2022. He was 9 months old. They are the first team in the United States to implant a patient with the angel stent.
“The angel stent is not a forever fix for most patients,” said Dr. McLennan. “But it is ideal for patients like Luis who need an intervention at a young age and who will need more procedures when they’re older. For Luis, we think the angel stent will keep the area open until it comes time for him to have a pulmonary valve replacement in 10-20 years. If not for the angel stent, we would have to bring Luis back every year or so to place a larger bare metal stent.”
A new future
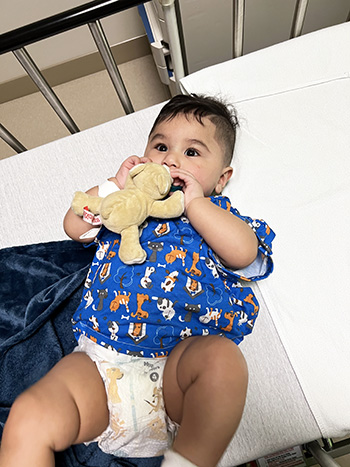
 Luis is now a happy, healthy 1-year-old who loves eating and is starting to walk. He’s had several follow-up appointments with Dr. Creighton and, so far, everything is right on track.
Luis is now a happy, healthy 1-year-old who loves eating and is starting to walk. He’s had several follow-up appointments with Dr. Creighton and, so far, everything is right on track.
“It’s such a team effort when it comes to taking care of our patients, whether it’s the surgeons, the outpatient team, or the inpatient team,” said Dr. Creighton. “One of the benefits of Children’s Wisconsin is that we have so many options to provide our patients with the best care and I’m so appreciative of the collaborative team effort here.”
Children’s Wisconsin is currently pursuing a first-in-the-country clinical trial for the angel stent.
“Our goal is to bring access to the most cutting-edge medicine to patients who need it,” said Jennifer Maldonado, a program manager from the Quality, Outcomes and Research Department at the Herma Heart Institute at Children’s Wisconsin. “We strive to be one of the most innovative centers in the country and we’re hoping to have 10-15 patients enrolled in a trial for the angel stent in the next 12 months.”
For Oneida and her husband, they’re just grateful for the chance they took and the care Baby Luis received.
“Everyone has been so good to us at Children’s Wisconsin,” said Oneida. “They always make you feel like everything is going to be okay even though it’s scary. There isn’t anywhere else you can go for access to this type of technology.”







