P
My name is Grace and I'm from Lincoln, NE.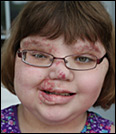
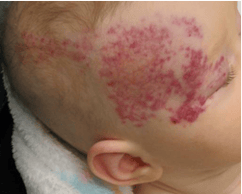
Kids like me who were born with PHACE Syndrome can have many different problems in different parts of their bodies. Each letter in P.H.A.C.E.S. stands for a different problem often found in this disease. I want to tell you a bit about the P in PHACE. P stands for Posterior fossa, which is the back part of the brain with the brainstem and cerebellum. I was born with a problem in how my brainstem grew as well as a cyst in that part of my brain. These problems affect my development and coordination, so I like coming to see the doctors at Children's Wisconsin who know a lot about PHACE Syndrome.
My PHACE looks like this:
P - I have problems with how my posterior fossa grew
H - I have a hemangioma on the right side of my head
A - I have arteries that don't work right because they are too small and not properly formed
C - My heart and some of the major arteries connected to it did not grow normally
E - I have vision problems because my eye did not form correctly
S
H
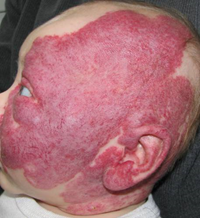
I'm London and I live in Wisconsin!
The most common thing you see in kids like me who have PHACE Syndrome is a big birthmark called a hemangioma on our heads and necks. That's what the H stands for in PHACE. When I was born, I had a hemangioma on my forehead, cheek, nose, and mouth. It started to grow, so my parents took me to Children's Wisconsin because the doctors knew how to help make sure my vision and breathing weren't harmed by getting me medication that helped keep the birthmark from growing too much. You can still see where my hemangioma was, but with my treatment helping to make it go away, I can see and breathe just fine!
My PHACE looks like this:
P
H - I have a hemangioma on my face and back
A - Many of the arteries in my neck did not grow properly
C - Parts of my heart grew in the wrong places
E
S
A
Hi, I'm EmmaLeigh from Bedford, IA.
Almost 75% of kids like me who have PHACE Syndrome have problems with the development of the arteries that carry blood from the heart up to the head and neck. The third letter in PHACE — the A — stands for Arteries. I have many arteries that grew either too big, too small, or grew in the wrong places. Doctors were able to fix some of the blood vessels that were pressing against my esophagus, the part of my throat I use to breathe and eat. My parents and my doctors are careful to make sure that my funny arteries don't give me any problems in the way I live and play by checking me with a special MRI designed for kids with PHACE.
My PHACE looks like this:
P - part of my posterior fossa is smaller than usual
H - I have a hemangioma on the right side of my head
A - Many of the arteries that carry blood to my brain are small or not developed correctly
C - Some of the blood vessels around my heart formed in the wrong places or grew incorrectly
E
S
C
My name is Eleanore and I live in De Pere, WI.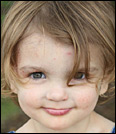
PHACE Syndrome can also cause kids like me to be born with problems with our hearts so that we need surgeries when we are very little! The C in PHACE stands for Cardiac problems, which means there are things wrong with development of the heart. When I was 2 years old I came to Children's Wisconsin to have a surgery on the big artery that comes out of my heart. I have two big scars from the surgery, but I'm feeling much better!
My PHACE looks like this:
P
H -I have a hemangioma on many places on my face and around my eye, on the side of my face and in my ear, and on my scalp and neck, too
A - On my neck, the artery on the right side is formed funny and doesn't work well
C - The big artery coming out of my heart did not grow properly and I needed surgery to help it out
E
S
E
Hello! I'm Elyse and I am from Chicago, IL.
Though not as common as some of the other problems seen in PHACE Syndrome, a few of us have problems with our eyes. The E in PHACE stands for Eye problems. One of my eyes has an optic nerve that is smaller than it should be. Because of this, I can't see properly out of that eye.
My PHACE looks like this:
P
H - My hemangioma covers my forehead and chin and I also have some inside my body, like on my stomach and spine
A - I have arteries that grew more twisty than normal
C - Some of the arteries coming out of my heart grew bulges and thin spots
E - One of my eyes is not formed correctly
S
S
I'm Lily and I live in Baden, PA!
The final letter in the PHACE Syndrome acronym is S which stands for problems with the Sternum. Some kids with PHACE Syndrome have sternal defects, which means the bone in the middle of your chest did not form correctly. Sometimes there are openings in the bone and sometimes there is scarring of the skin over the middle of the chest. I was born with a bump on my sternum bone which looks like a scar in the front of my chest. I travel to Milwaukee each year to have the doctors at Children's Wisconsin check how I'm doing.
My PHACE looks like this:
P
H - I have a hemangioma on my lower face and upper chest
A - Many of the arteries in my neck did not grow properly
C - parts of my heart grew in the wrong places
E
S - I have a scar on my chest where my sternum grew differently than normal