Just like fingerprints, no two people are exactly alike. Take, for example, Caleb and his twin brother, Tyler. Born in 2006, Caleb had a rare congenital heart defect (CHD) — a double outlet right ventricle, single ventricle variant — while Tyler had no such defect. When parents, Chris and Stephanie, became pregnant again in 2009, doctors discovered the baby girl also had a CHD — another single ventricle disease. Emma was born in January 2010 and officially diagnosed with hypoplastic left heart syndrome.
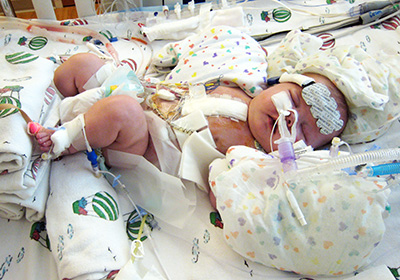 A single ventricle heart defect is a condition where one of the two pumping chambers in the heart (ventricles) doesn’t develop properly, resulting in oxygen-poor blood being pumped throughout the body. Single ventricle defects can be several varieties and affect about one in 4,000 live births in the United States and worldwide. Single ventricle defects are among the most common complex heart problems yet one of the most debilitating. They typically require a series of surgeries referred to as, “the single ventricle pathway.” For example, in the case of hypoplastic left heart syndrome, three open-heart surgeries — the Norwood, Glenn and Fontan — are required beginning typically during the first week of life and completing at about three years of age.
A single ventricle heart defect is a condition where one of the two pumping chambers in the heart (ventricles) doesn’t develop properly, resulting in oxygen-poor blood being pumped throughout the body. Single ventricle defects can be several varieties and affect about one in 4,000 live births in the United States and worldwide. Single ventricle defects are among the most common complex heart problems yet one of the most debilitating. They typically require a series of surgeries referred to as, “the single ventricle pathway.” For example, in the case of hypoplastic left heart syndrome, three open-heart surgeries — the Norwood, Glenn and Fontan — are required beginning typically during the first week of life and completing at about three years of age.
In Caleb’s case, because of his specific anatomy, he was able to avoid immediate intervention after birth. Instead of having the Norwood procedure, Michael Mitchell, MD, surgical director at the Herma Heart Institute at Children’s Wisconsin, performed a pulmonary artery banding surgery when Caleb was 3 months old. Four months later, Dr. Mitchell performed Caleb’s Glenn procedure, followed by the Fontan when Caleb was 3 years old.
Emma’s journey with hypoplastic left heart syndrome was more challenging. In addition to the Norwood, Glenn and Fontan, she required additional work on her pulmonary veins and tricuspid valve. Emma was even placed on the heart transplant list at 9 months, but after her Fontan procedure and tricuspid valve repair at age 5, she improved enough to be removed from the transplant list.
Next-level research
 Not too long ago, most patients with a single ventricle defect would die shortly after birth. Today, the majority of them not only survive, but are living well into their 30s and even beyond thanks to medical advancements.
Not too long ago, most patients with a single ventricle defect would die shortly after birth. Today, the majority of them not only survive, but are living well into their 30s and even beyond thanks to medical advancements.
For Dr. Mitchell, Joy Lincoln, PhD, director of cardiovascular research at the Herma Heart Institute, and Aoy Tomita-Mitchell, PhD, a cardiac researcher at the Children's Research Institute and professor of cardiothoracic surgery and biomedical engineering at the Medical College of Wisconsin, the clinical goal is not just ensuring patients survive surgery, but to help patients live as normal a life as possible. One way they’re doing that is through cardiac precision medicine.
Precision medicine looks at genetics, environment and lifestyle to better determine the most appropriate treatment option for affected individuals. In many cases, clinical and research teams will use genetic information and a patient’s own cells to guide personalized treatment solutions. At Children’s Wisconsin, it involves a multi-disciplinary approach to understanding the cause and development of disease for each child, and outlining the most effective treatment plan. This work is made possible in large part due to the affiliation with the Medical College of Wisconsin.
The Medical College of Wisconsin has been the academic partner of Children’s Wisconsin since 2000. As an academic medical center, Children’s Wisconsin is able to set quality standards for patient care nationwide, train the health care workforce and further scientific concepts through research and clinical trials. In short, this means families get the best care possible for their children.
“Caleb, Tyler and Emma have the same parents, but experienced three different cardiac outcomes at birth,” said Dr. Lincoln. “The typical approach to medicine has been to take the ‘one size fits all’ treatment strategy, but this does not benefit everyone. We tailor-make suits to fit the individual wearing them, so for the same reason, we should tailor treatment plans for each person’s disease or defect.”
The Cord Blood Program is one type of cardiac precision medicine. It was established in 2019 by Dr. Lincoln with the help of Dr. Mitchell and Dr. Tomita-Mitchell. Umbilical cord tissue and blood is a highly enriched source of stem cells, which have the ability to differentiate into specialized cell types depending on the environment they’re cultured in, including those of the heart and other cardiovascular structures. The ultimate goal is to bank umbilical material from patients at the time of delivery and strive to use the patient’s own stem cells to generate the necessary heart cells or structures that each patient may need to improve their outcome and quality of life.
“Using the child’s own cells to create surgical material to rebuild their heart would help overcome rejection limitations and potentially negate the need for lifelong medication to prevent clots, which is required when devices like pacemakers, stents and animal or artificial valves are used,” said Dr. Lincoln. “We may also prevent or avoid the need for a heart transplant.”
The cord blood bank allows for the clinical grade storage of umbilical cord tissue and blood for families at no cost to them, whether their child has a CHD or not. By participating in the program, the cord blood and tissue is used by the Herma Heart Institute’s research team to explore the cause of CHDs and develop new therapies and treatments, and is available for families to retrieve at any time.
While the Cord Blood Program is focused on the heart right now, there are infinite uses of stem cells to benefit children affected by other diseases in the future, including pediatric cancer and other rare childhood diseases.
“Our precision medicine team continues to grow and includes research scientists, biomedical engineers, molecular biologists, geneticists, surgeons, cardiologists and more,” said Dr. Lincoln. “We are very fortunate to have such highly qualified team members within the Herma Heart Institute who are willing to invest their careers in making personalized medicine a reality.”
The future of heart treatment
 Caleb, Tyler, Emma and their parents, Chris and Stephanie, have been research participants at the Herma Heart Institute since Emma was an infant.
Caleb, Tyler, Emma and their parents, Chris and Stephanie, have been research participants at the Herma Heart Institute since Emma was an infant.
“We actually pursued the research because of our uncommon family history,” said Chris. “We were very passionate about getting involved because we were hoping our situation could improve outcomes for future kids. We never thought it might help our own kids.”
For Chris, it’s been fascinating to see the advancements in CHD research and care over the last 12 years.
“It’s remarkable how rapidly Children’s Wisconsin has been able to make progress and advancements that really impact how kids are treated and improve the quality of their lives,” said Chris. “We really don’t know if our kids will need a heart transplant. Early on, doctors told us, ‘Ultimately a transplant will be needed.’ But as medicine continues to evolve, who knows what will happen. We’re really excited to see where precision medicine goes.”
Expecting families at risk of developing a CHD, or with infants diagnosed with a disease prior to delivery, are encouraged to discuss the Cord Blood Program with their fetal care team, physician or by completing this form. Participation is not limited to patients of Children’s Wisconsin or the Herma Heart Institute, and healthy pregnancies are encouraged to participate as well.







