In this section
Our areas of focus
- Adult Congenital Heart Disease Program
- Our ACHD specialists
- ACHD webinar series
- Pregnancy and ACHD
- Frequently asked questions
- Advanced Diagnostics
- Cardiac Anesthesiology
- Cardiogenetics Program
- Cardiac Catheterization
- Cardiac Intensive Care Unit
- Cardiac Physical Activity Program
- Cardiac precision medicine
- Cord blood program
- Developmental Follow-up Program
- Educational Achievement Partnership Program
- Electrophysiology Program
- Fetal Heart Program
- Fontan Survivorship Program
- General Cardiology
- Healthy Hearts Program
- Heart healthy eating
- Heart Failure Program
- Heart Surgery
- Heart Transplant
- Home Monitoring Program
- Marfan Syndrome Program
- Project ADAM
- Pulmonary Hypertension
- Tracheal Disorders Program
- VAD and ECMO Program
Jenni's story and the importance of ACHD checkups

It was a late night in December 2007 and 37-year-old Jenni Sego was at work when a coworker who was training to be a nurse asked to take her blood pressure to practice. Jenni said sure.
“I knew it was going to be high. I work third shift, I have three kids and I don’t sleep,” said Jenni. “She took it multiple times and it kept coming back 200/100. I just kept making up excuses because I felt fine. She said I really needed to go to the doctor.”
It had been a long time since Jenni had seen a doctor, but when she was a child she was in and out of doctors’ offices all the time. Born with primum atrial septal defect and a cleft mitral valve (a hole between the two upper chambers of her heart and a gap in her mitral valve), Jenni underwent heart surgery at Children’s Wisconsin when she was 4 years old.
After that surgery, life went on pretty much as normal.
“I did everything you do as a kid. My mom never treated me as if I was different or special or couldn’t do things,” Jenni said. “As far as I knew everything was going well. That’s my problem. That’s what scares my husband. I don’t know what bad feels like.”
Healthcare limbo
As Jenni entered adulthood, she didn't realize she was moving into a health care no man's land. By the time her coworker took her blood pressure that night, she hadn't seen a cardiologist in nearly 20 years. Unfortunately, her story is all too common.
Prior to about 1944, most children born with congenital heart disease simply didn't survive. Even in the late 1980s, the percentage of children born with severe cardiac defects who died within the first year of life was 25 percent. Today that figure is less than 5 percent.
Thanks to medical advances and new surgical procedures, people born with congenital heart disease are now living into adulthood. In the United States, there are an estimated 1.4 million adults living with congenital heart disease and they require unique, lifelong medical care and management.
The problem is pediatric cardiologists, by definition, aren't trained to care for the needs of an adult patient. At the same time, since congenital heart disease is different than heart disease that is acquired by age or lifestyle factors, most adult providers and cardiologists aren't trained to care for it.
The result is a lack of adult cardiac physicians who are trained to treat congenital heart disease. In fact, there wasn't even an official certification for adult congenital heart disease specialists until early 2016.
That is why in 2004 the Adult Congenital Heart Disease Program was created at the Herma Heart Institute, the first in Wisconsin and one of the first in the nation.
Comprehensive adult medical care

At the urging of her family and co-worker, Jenni finally saw an adult congenital cardiologist in the Herma Heart Institute in March 2008. It was almost a four-hour appointment.
He asked how many kids she had — three. He asked how many pregnancies — four. He asked if her babies were full term, healthy weight — yes. He then paused for a moment and told Jenni that she must have somebody upstairs watching over her.
Her doctor went on to explain that Jenni had coarctation of the aorta — meaning the main artery that provides blood to her body was severely narrowed.
"He said I was born with this and it's something that is usually repaired as a child," said Jenni. "He said I was a heart attack waiting to happen."
There were times in her life where Jenni would become so out of breath she would be forced to stop what she was doing — shoveling, for example. But Jenni jokes she always thought she was out of shape — even though she exercises seven days a week — and she'd just get right back to it.
After that initial meeting, Jenni became a regular visitor to the Herma Heart Institute's Adult Congenital Heart Disease Program.
In June 2008, she had surgery to repair her narrowed artery.
In April 2009, the electrical connections between the top and bottom of her heart stopped working (atrial tachycardia) and she underwent another surgery.
In April 2017, she developed an irregular heartbeat (atrial flutter).
In July 2017, she underwent a procedure in which her heart was shocked back into rhythm (cardioversion). Following that procedure, all three of her heart's internal pacemakers stopped functioning (known as complete heart block), so the next day she was fitted for a pacemaker.
"After my pacemaker, I told my husband I'm never dying," Jenni joked. "I have a bionic heart, I'm going to live forever."
In addition to the wide array of medical services Jenni received, the Adult Congenital Heart Disease Program also provides a full range of psychosocial services as well.
The program is 100 percent dedicated to meeting the comprehensive needs of adult survivors of congenital heart disease— not only the medical needs, diagnostic needs, and the surgical needs of our patients but also all their social and psychological needs.
No place she'd rather go
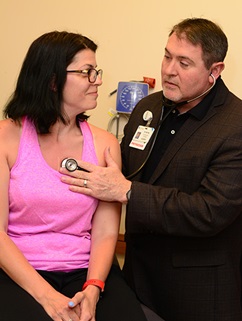
After Jenni checks in for her bi-annual appointment at the Herma Heart Institute at Children's, she takes a seat in the waiting room beside a TV playing a Curious George cartoon.
Below the TV is a wooden bookshelf overflowing with colorful books about trucks and dinosaurs and farm animals. A couple chairs down a father comforts his crying son, rocking him gently in his arms. In the far corner, a little girl sits at a small red table coloring in a picture of a smiling fish.
After a few minutes, a nurse calls Jenni's name and walks her back to the exam room. A few hours later, she receives a clean bill of a health and will be back to see her cardiologist in six months.
Everyone knows Children's is the only hospital in the area dedicated solely to children, but many are often surprised to learn and wonder why it also has one of the nation's largest adult heart programs, too.
"I still ask myself to this day — I'm an adult, why do I go to Children's," said Jenni. "People ask me that. I say that's where I started, that's where my history is and they have an adult program. There's no place else I would go."
